“ Abstract This educational post explores the transformative impact of Glucagon-Like Peptide-1 (GLP-1) receptor agonists in the management of metabolic diseases, including obesity and type…


“ Abstract This educational post explores the transformative impact of Glucagon-Like Peptide-1 (GLP-1) receptor agonists in the management of metabolic diseases, including obesity and type…

Platelet-Rich Plasma Therapy: Dosing and Clinical Use Abstract As a clinician deeply invested in integrative and regenerative medicine, I am continually fascinated by the body’s…

“ Abstract In this educational post, I walk you through how I evaluate and manage common musculoskeletal pain conditions in athletes and active individuals using…

Memorial Day Rear-End Injury Chiropractic Recovery Memorial Day weekend means exciting road trips, beach days, and family cookouts for many people in El Paso and…

Uncover the role of hormonal health in promoting patient wellness and enhancing quality of life for the body. Abstract Welcome to our educational series. I’m…

PRP Therapy for Injury Recovery and Joint Support Abstract Welcome to our educational journey into the world of regenerative medicine, with a focus on Platelet-Rich…

PRP and Chiropractic Care for Musculoskeletal Healing Abstract In this educational post, I walk you through the modern science of platelet-rich plasma (PRP) from a…

“ Abstract As a clinician dedicated to providing the most advanced and effective treatments, I am constantly navigating the complex world of regenerative medicine. This…

Old Car Accident Pain Relief with Advanced Therapies Many people walk away from a car crash thinking the worst is over. Months or even years…
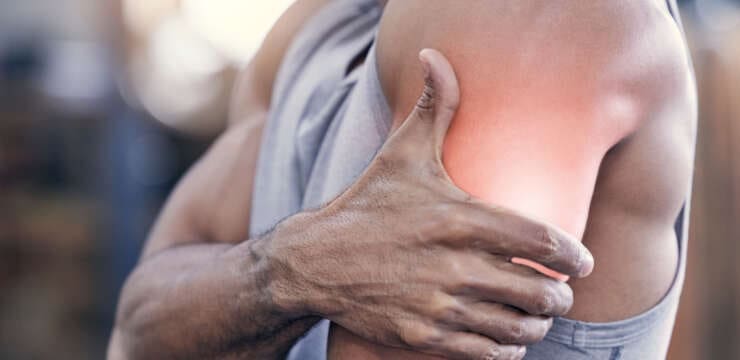
Explore how orthobiologics can transform regenerative medicine approaches for better outcomes in musculoskeletal health. Abstract In this educational post, I walk you through the current…
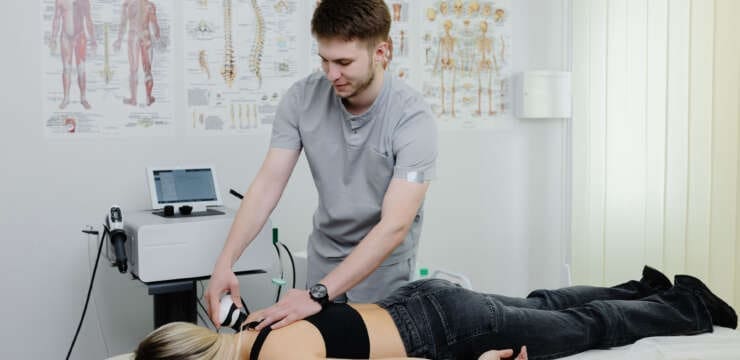
MLS Laser Therapy for Pain Relief, Healing, and Recovery Abstract In this educational post, I will guide you through the sophisticated world of Multiwave Locked…
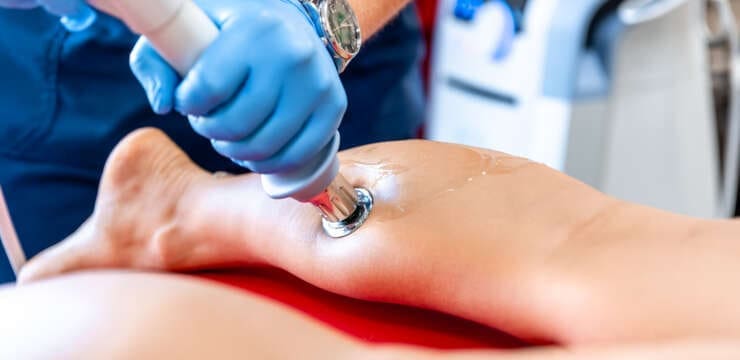
Learn how therapeutic approaches that use photobiomodulation can aid tissue regeneration and shorten recovery times. Abstract In this educational post, I will guide you through…

Chiropractic and Regenerative Healing After a Crash Motor vehicle accidents (MVAs) can leave your body with lasting pain and limited movement. Soft tissue damage, ligament…
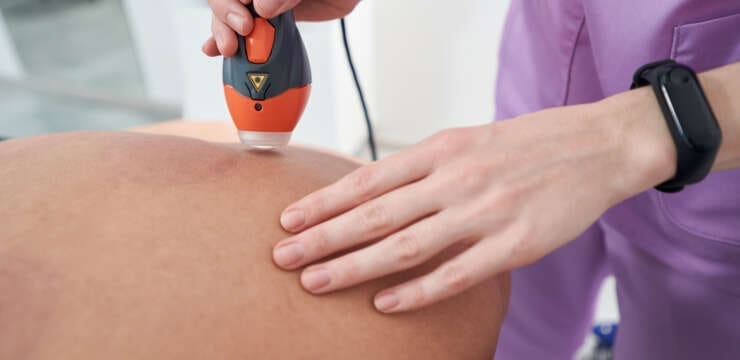
Discover how MLS laser therapy, combined with photobiomodulation, can effectively enhance recovery and reduce inflammation. Abstract As a practitioner dedicated to integrative and functional medicine,…
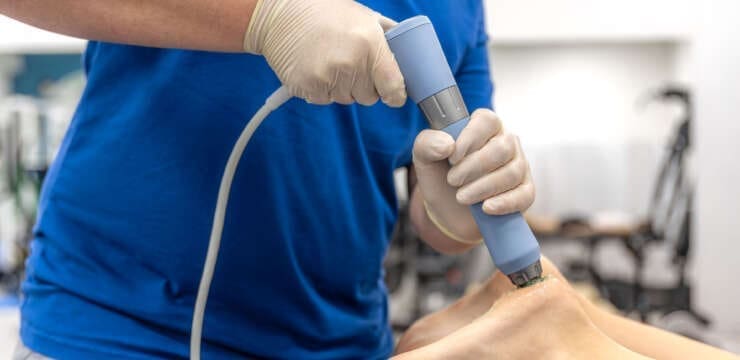
Orthobiologics, Shockwave, and Chiropractic Healing Abstract In this educational post, I share a first-person journey from debilitating plantar fasciitis to lasting recovery with electrohydraulic shockwave…

Learn about ultrasound therapy and its role in improving treatment outcomes for musculoskeletal injuries in the body. Abstract As a practitioner dedicated to integrative and…
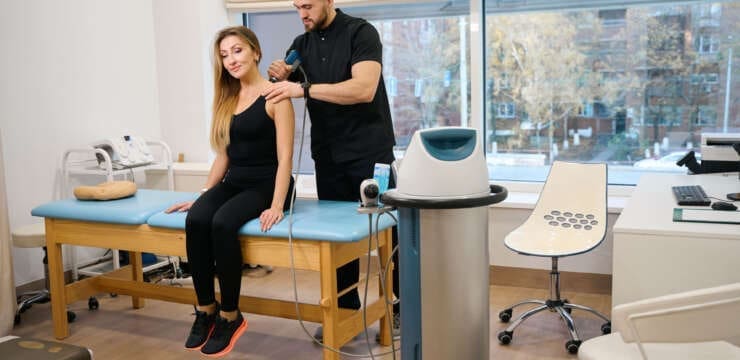
Shockwave Therapy for Natural Musculoskeletal Healing and Regeneration Abstract As a Doctor of Chiropractic and a board-certified Family Nurse Practitioner, I am constantly exploring innovative,…