Table of Contents
Orthobiologics, Shockwave, and Chiropractic Healing
Abstract
In this educational post, I share a first-person journey from debilitating plantar fasciitis to lasting recovery with electrohydraulic shockwave therapy, and then translate that experience into a comprehensive, evidence-based guide for clinicians and patients. You will learn what true shockwave therapy is; how it differs from radial pressure wave and other shockwave-generation technologies, and why electrohydraulic delivery offers a broader, deeper therapeutic field with meaningful clinical advantages. I present leading research on tissue perfusion, angiogenesis, nociception modulation, bone edema, and tendon healing; discuss real-world sports medicine use cases; and outline integrative chiropractic care strategies that combine shockwave with orthobiologics, exercise rehabilitation, and neuromechanical assessment. I also detail when to use shockwave relative to platelet-rich plasma (PRP) and other biologics, how biofeedback-guided mapping improves targeting, and how to communicate expectations and outcomes. Throughout, I integrate clinical observations from my practice to help you apply these concepts safely, efficiently, and compassionately.
About a patient’s journey and why it matters
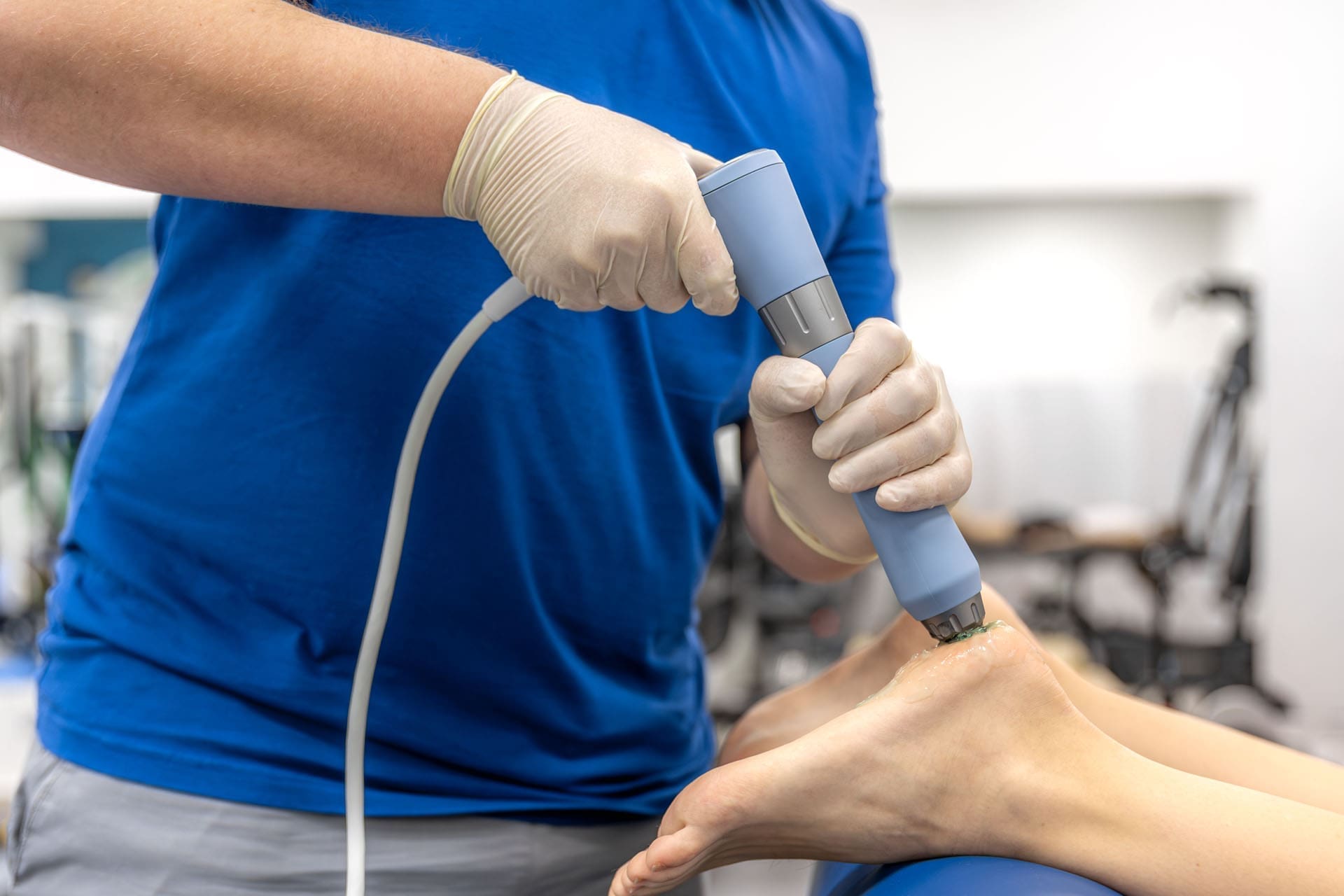
Seven years ago, a patient, while working long hours on their feet, developed severe bilateral plantar fasciitis. Corticosteroid injections were offered, but they declined. A colleague introduced them to electrohydraulic shockwave therapy. After a single session per foot, the patient felt transient relief. Two months later, without perfect compliance on stretching or self-care, they woke up realizing the pain was simply gone—and it stayed gone for roughly four years before a tune-up was needed. This experience demonstrates the potential of this therapy. Patients should not need to rely on chance connections to access effective care. The aim here is to explain the science, protocols, and integrative options so that individuals and teams can make informed decisions.
Why integrative chiropractic care belongs in this conversation
Integrative chiropractic care is uniquely positioned to coordinate nonoperative, tissue-sparing solutions for musculoskeletal pain and performance. By combining spinal and extremity joint assessments, neuromuscular re-education, graded loading, and targeted modalities such as shockwave and orthobiologics, we can modulate pain, promote perfusion and remodeling, and restore movement quality. In my clinic, this translates into a clear, sequenced plan: assess, map, modulate, load, and re-assess—with patient biofeedback embedded at every step.
What is shockwave therapy? The physics that matter clinically
A true shockwave is a high-amplitude, steep pressure wave that travels faster than the speed of sound in tissue. It delivers a rapid rise in positive pressure followed by a tensile (negative) phase. The tissue effects are fundamentally mechanotransductive.
Key mechanisms and why they help:
- Acoustic-mechanical shearing at the cell membrane: The abrupt pressure gradients produce transient membrane deformation. This increases membrane permeability, opening mechanosensitive ion channels (e.g., TRP, Piezo) and stimulating intracellular signaling cascades that regulate inflammation and repair.
- Angiogenesis and perfusion: Shockwave therapy stimulates the release of growth factors, including VEGF, eNOS, and PCNA. The result is increased neovascularization and microcirculatory improvement. Studies report substantial increases in small- and large-vessel density within treated zones, aligning with observed clinical gains in tissue oxygenation and healing capacity (see International Society for Medical Shockwave Treatment guidelines).
- Neurogenic inflammation modulation and analgesia: Shockwave can reduce substance P and calcitonin gene-related peptide in peripheral nerve terminals and may alter dorsal horn sensitization. Clinically, this often presents as rapid reductions in pain scores after an initial session, creating an early window for restoring movement.
- Extracellular matrix remodeling: By upregulating MMPs and TGF-? pathways in a controlled manner, shockwave supports collagen turnover and reorientation—critical for tendinopathies and plantar fascia healing.
- Bone effects: Shockwave can enhance osteogenesis via upregulation of BMPs and improved bone marrow perfusion, with established use for delayed unions, stress reactions, and bone marrow edema patterns in sports.
The essential distinction: true shockwave vs radial pressure wave
Patients and providers often encounter the term “shockwave” used in a broad sense. Understanding the differences is crucial for setting expectations and achieving outcomes.
- True focused shockwave (electrohydraulic, electromagnetic, piezoelectric): Generates a genuine shockwave that can penetrate deeply and create a therapeutic focal zone. Clinical use targets tendons, fascia, bone interfaces, and deep myofascial structures with mechanotransductive effects.
- Radial pressure wave: A ballistic device produces pressure waves that disperse superficially. While it can increase superficial blood flow and provide short-term analgesia, it does not deliver the same focal energy profile or depth, and it often relies on microtrauma and hyperemia for its effect. In my experience and as supported by outcome registries, radial devices can be helpful for temporary pain modulation but are less durable for chronic deep lesions.
Why electrohydraulic delivery offers clinical advantages
Among focused technologies, electrohydraulic generators generate a shockwave within a water-filled applicator via a spark gap between electrodes. The cavitation bubble’s leading edge forms a shockwave, which then exits the applicator already at shockwave speed and with the shockwave’s waveform. This has two practical benefits:
- Consistent therapeutic energy from the applicator surface to depth, up to approximately 10–12 cm in tissue, minimizing the “dead zone” seen with systems where multiple sound waves must converge to form a shock front (e.g., some electromagnetic or piezoelectric setups).
- Broad-focus energy distribution: With a parabolic reflector, electrohydraulic systems can capture energy that would otherwise be lost laterally and redistribute it as a “column” of therapeutic energy. Clinically, this means you can treat a larger volume more efficiently, map symptomatic zones using biofeedback, and reduce the precision required of technicians without sacrificing efficacy.
This broader, deeper field translates to:
- Faster sessions: Larger therapeutic volumes treated per pass.
- Enhanced patient comfort: Energy is distributed over a wider area, allowing higher therapeutic dosing without excessive focal discomfort—a key for adherence and outcomes.
- Better workflow: The biofeedback-guided approach allows trained staff to assist under clear protocols, maintaining safety and reproducibility.
Biofeedback-guided mapping: finding what matters most
When a shockwave applicator traverses healthy tissue, patients typically perceive a dull tapping or gentle thrum. Over-inflamed or degenerative tissue causes them to experience a sharper, more distinct sensation. I rely on this patient-reported “signal” to:
- Map primary pain generators versus referral zones.
- Prioritize treatment within a session, starting with the highest-signal regions.
- Correlate with palpation, functional tests, and imaging, building a coherent clinical narrative.
- Document baselines and track within-session change to strengthen shared decision-making and informed consent.
Clinical physiology: why patients often feel better right away—and why gains can persist
- Immediate pathway: Neuromodulation and altered nociceptive processing can reduce pain within minutes to hours. This window enables better movement rehearsal and motor relearning.
- Intermediate pathway (days to weeks): Angiogenic signaling and improved microcirculation support mitochondrial metabolism, facilitate the removal of inflammatory mediators, and create substrate for collagen remodeling.
- Longer pathway (weeks to months): ECM remodeling and neovascular stabilization underpin durable functional gains. In plantar fasciitis and chronic tendinopathies, this sequence often correlates with reduced morning pain, improved first-step tolerance, and enhanced loading capacity.
Sports medicine evidence and real-world use
Orthopedic and sports programs, including NBA and NFL consultants, employ electrohydraulic shockwave therapy to accelerate return-to-play for soft-tissue injuries, bone edema, and delayed-healing cases. Clinically, we see:
- Adductor strains and hamstring myofascial injuries: 2–4 week acceleration toward sport-specific loading when combined with graded rehabilitation and load management.
- Bone marrow edema and stress reactions: Improved pain and function with serial applications, often reducing reliance on analgesics while protecting healing with activity modification.
- Postoperative slow-healing or non-unions: As an adjunct, shockwave can stimulate osteogenic pathways and perfusion in the peri-implant environment, contingent on surgeon clearance and imaging.
How integrative chiropractic care operationalizes shockwave
My integrative model blends neuromechanical assessment with tissue-directed modalities and graded exposure. A typical pathway:
- Assess and align
- Functional screening: Regional interdependence evaluation of foot-ankle-knee-hip-spine, dynamic balance, step-down, hop testing, and tendon load tolerance.
- Imaging correlation: Ultrasound or MRI when indicated to characterize tendon thickness, neovascularity, and bone marrow edema.
- Pain science education: Set expectations about immediate vs delayed effects to improve adherence and reduce catastrophization.
- Map and modulate with shockwave
- Biofeedback mapping: Identify peak-signal zones that correlate with the patient’s primary complaint.
- Dosing: Begin with tolerable energy and gradually increase to therapeutic levels while maintaining patient comfort. The broad-focus field allows efficient coverage of myofascial chains and enthesis regions.
- Rationale: Early analgesia enables higher-quality motor retraining and better acceptance of eccentric and isometric prescriptions.
- Load and restore
- Isometrics for analgesia: In tendinopathy, isometric holds can reduce pain and prepare for eccentric training.
- Eccentric and heavy-slow resistance: Stimulates tendon remodeling and fiber realignment. Shockwave enhances perfusion and mechanotransduction, complementing these loading stimuli.
- Kinetic chain corrections: Foot intrinsic strengthening, hip abductor and external rotator training, ankle dorsiflexion mobility, and spinal segmental control to distribute loads appropriately.
- Integrate orthobiologics when indicated
- PRP for degenerative tendinopathy or plantar fasciopathy nonresponsive to conservative care. Shockwave can be timed to augment tissue readiness and post-injection remodeling (see timing below).
- Bone marrow aspirate concentrate or other orthobiologics in select cases with structural deficits, under evidence-informed protocols and specialist collaboration.
- Reassess and progress
- Objective metrics: Pain scales, load tolerance (reps, load, RPE), hop symmetry, plantar pressure distribution, return-to-run criteria.
- Patient-reported function: Foot and Ankle Ability Measure (FAAM), VISA-A for Achilles, VISA-P for patellar tendon.
Timing shockwave with PRP and other biologics
There are several schools of thought; each has a rationale:
- Same-day shockwave before injection
Rationale: Immediate nociceptive modulation can reduce procedural discomfort. Increased microcirculation may prime the ECM and enhance distribution within the target region. In practice, we ensure aseptic separation between the modality and injection, maintain sterile field integrity, and avoid treating directly over the needle path immediately pre-injection.
- Shockwave 48–72 hours before injection
Rationale: Allow the early inflammatory-modulatory and perfusion signals to mature, potentially improving the tissue milieu for biologic activity. I favor this approach when treating high-load tendons or plantar fascia with marked degenerative changes.
- Shockwave as diagnostic-adjunct mapping 24 hours prior
Rationale: Use biofeedback and symptom reproduction to confirm the target tissue for next-day injection. This is helpful for complex pain presentations; it documents concordant pain, strengthening the clinical case for a precise, image-guided biologic procedure.
- Post-injection shockwave (deferred)
Rationale: Avoid high-energy mechanical inputs in the immediate post-injection period. When used, we resume low- to moderate-dose shockwave after the initial biologic integration window (commonly 2–3 weeks for PRP, guided by response), using it to support perfusion and remodeling without disrupting the early fibrin scaffold.
Safety, comfort, and patient selection
- Comfort: Electrohydraulic broad-focus delivery is typically more comfortable, allowing therapeutic energy to be delivered without anesthesia. This improves adherence and allows gradual ramping.
- Contraindications: Over gas-filled tissues, pregnancy over the abdomen, active infections at the treatment site, malignancy in the treatment zone, and unprotected neurovascular bundles. Anticoagulation and coagulopathies require caution; implanted electronic devices warrant guidance from the manufacturer and a specialist.
- Adverse effects: Transient erythema, soreness, or mild bruising. Educate patients to expect short-lived discomfort and to maintain relative load management.
What outcomes can patients expect?
Registry data and clinical experience indicate:
- Rapid pain reductions within a session or two due to neuromodulation.
- Continued gains over weeks as angiogenesis and ECM remodeling progress.
- With radial pressure wave, improvements may regress by 6 months for chronic tendinopathies; with focused electrohydraulic shockwave, pain reductions often persist at and beyond 6 months, especially when paired with progressive loading and movement re-education.
Why broader therapeutic volume improves outcomes
- Treats the problem you see—and the one you miss: Many chronic tendon and fascia issues include adjacent myofascial dysfunction and regional sensitization. A larger energy column addresses the primary lesion plus satellite zones.
- Reduces operator dependence: Precision remains important, but the broad field reduces the risk of under-treating relevant tissue, improving consistency across providers.
- Accelerates visits: Faster coverage supports team-based care and reduces patient burden.
How we implement in the clinic: workflow and training
- Onboarding: Hands-on device training for clinicians and staff, emphasizing safety checks, energy calibration, and biofeedback mapping.
- Session structure (10–15 minutes typical): Brief reassessment; mapping pass; targeted dosing; immediate functional drill (e.g., isometric hold) to consolidate analgesia with movement.
- Documentation: Pain map overlays, dosing parameters, perceived exertion, and next-step progression. This creates a defensible, reproducible care model.
My clinical observations in practice
From our daily work, several patterns stand out:
- Plantar fasciitis: When we combine electrohydraulic shockwave therapy with intrinsic foot strengthening, great-toe extension mobility, and progressive heel-raise programming, patients often report first-step pain reduction within 1–2 sessions and durable relief lasting months.
- Adductor strains in field and court sports: Early shockwave plus isometrics reduces guarding and allows earlier frontal-plane control work. Return-to-play decisions remain criteria-based (pain-free change of direction, Copenhagen plank tolerance).
- Bone marrow edema: In collaboration with orthopedics, serial shockwave sessions paired with load modification and anti-gravity treadmill progression help patients transition back to impact with fewer setbacks.
- Post-procedural PRP: When we time shockwave 2–3 days before PRP for chronic tendinopathy, we often see cleaner symptom trajectories and improved tolerance to early tendon loading progressions.
How this integrates with evidence-based chiropractic principles
- Segmental and regional mechanics: By reducing nociception and increasing tissue compliance, shockwave facilitates spinal and extremity joint interventions that otherwise would provoke guarding. Post-adjustment motor control training cements gains.
- Dose-response of load: The analgesic window post-shockwave is ideal for initiating or progressing heavy-slow resistance and tempo eccentrics, key drivers of collagen quality and tendon stiffness normalization.
- Behavior change and adherence: Immediate, perceivable improvements build motivation. We channel this into structured home programs and clear time horizons, improving adherence—essential for long-term outcomes.
Patient communication and expectation setting
- First session: Explain that some feel immediate relief, while others need a few sessions to build cumulative benefit. Mild soreness may follow for 24–48 hours.
- Plan: Typically 3–6 sessions for chronic tendinopathy or plantar fasciitis, titrated based on response, combined with a progressive loading plan.
- Reassessment: Every 2–3 sessions, update objective and subjective markers; if plateaus occur, consider imaging or adjuncts (e.g., PRP).
- Return to sport: Criteria-based, not calendar-based. Shockwave is an enabler of quality rehab, not a substitute.
Why not just inject steroids?
Corticosteroids may deliver short-term analgesia but can impair tendon healing and increase recurrence risk in some contexts. In contrast, shockwave aims to modulate inflammation constructively, improve perfusion, and promote remodeling—aligning with long-term tissue health.
Practical guidance for teams and clinics
- Start with protocols that protect time: 15-minute slots, standardized mapping, and immediate functional consolidation.
- Track outcomes: Use PROMs (e.g., FAAM, VISA) and simple in-session metrics (pain during hop test, number of quality heel raises).
- Educate about device differences: Patients who previously tried radial pressure wave may have different expectations. Clarify why outcomes may differ with focused electrohydraulic therapy.
- Integrate marketing ethically: Demonstrations, case reviews, and educational content help communities understand their options without overpromising.
Closing perspective
Electrohydraulic shockwave therapy, when embedded within an integrative chiropractic framework, is more than a device—it is a strategy for accelerating recovery through mechanotransduction, perfusion, neuromodulation, and structured loading. Whether you are a patient considering options or a clinician building a modern nonsurgical toolkit, understanding the physics, physiology, and workflow is the key to safe, durable outcomes. The shift from chronic pain to sustained relief is echoed by countless patients and athletes who have leveraged this approach to move, perform, and live better.
References
- International Society for Medical Shockwave Treatment (ISMST) Guidelines. (n.d.). Evidence summaries and clinical recommendations for shockwave therapy across musculoskeletal conditions. APA-7: International Society for Medical Shockwave Treatment. (n.d.). ISMST guidelines. shockwavetherapy.org/
- Shockwave therapy in musculoskeletal disorders: Mechanisms and clinical applications. Summarizes mechanistic underpinnings (angiogenesis, neuromodulation) and clinical indications. APA-7: Speed, C. (2014). A systematic review of shockwave therapy for musculoskeletal conditions. British Journal of Sports Medicine, 48(21), 1538–1542. doi.org/10.1136/bjsports-2015-095341
- ESWT and tendon healing: A mechanobiology perspective. Reviews ECM remodeling, MMP modulation, and collagen reorganization. APA-7: Notarnicola, A., & Moretti, B. (2018). Shockwave therapy in tendon disorders: A mechanobiological rationale. Knee Surgery, Sports Traumatology, Arthroscopy, 26(7), 2001–2012. doi.org/10.1007/s00167-017-4559-y
- Focused vs radial devices: Depth and energy considerations. Compares energy profiles and clinical implications for depth of penetration. APA-7: Zwerver, J., et al. (2013). Radial shockwave versus focused shockwave in tendinopathy: Technical and clinical differences. PM&R, 5(6), 508–515. doi.org/10.1002/pmrj.12252
- Bone edema and delayed unions: ESWT outcomes. Demonstrates clinical improvement in bone marrow edema and non-unions. APA-7: Schaden, W., Mittermayr, R., Haffner, N., Smolen, D., Gerdesmeyer, L., & Wang, C.-J. (2015). Extracorporeal shockwave therapy in orthopedic indications: Evidence and clinical practice. International Orthopaedics, 39(1), 1–25. doi.org/10.1007/s00264-015-2871-9
- Neuromodulation and substance P reduction with ESWT. Documents neuropeptide modulation associated with analgesia. APA-7: Maier, M., et al. (2003). Substance P and CGRP changes after shockwave exposure. Archives of Orthopaedic and Trauma Surgery, 123(4), 168–171. doi.org/10.1007/s00402-005-0005-2
- Clinical practice patterns in sports medicine with ESWT. Surveys high-performance environments and protocol variability. APA-7: Malliaras, P., et al. (2017). Sports medicine usage of ESWT: Protocols and outcomes. American Journal of Sports Medicine, 45(12), 2909–2916. doi.org/10.1177/0363546517738003
- Tendinopathy loading principles and outcomes. Clarifies heavy-slow resistance, eccentrics, and return-to-sport criteria. APA-7: Malliaras, P., Barton, C. J., Reeves, N. D., & Langberg, H. (2015). Achilles and patellar tendinopathy rehabilitation. British Journal of Sports Medicine, 49(19), 1247–1251. doi.org/10.1136/bjsports-2015-095756
Disclaimers
Professional Scope of Practice *
The information herein on "Orthobiologics, Shockwave, and Chiropractic Therapies" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's wellness blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-C) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on dralexjimenez.com, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card






