
We’ve said it before, we all have reactions to food and food disturbances. Adverse food reactions had become one of the most common doctor’s office visits. In a study performed in the United Kingdom, 20% of the population reported having a food intolerance, and in Germany, one-third of the population studied reported having reactions to food. When placebo-controlled challenges were done, it turned out that less than 2% of the UK studied population resulted in food intolerance. Similarly, only 3.6% in the German study presented an adverse reaction to food. Current information shows that women are more common to self-perceived food adverse reactions when compared to men. Could it be possible that we don’t know what our bodies are reacting to? Let’s dive in and find out about adverse food reactions, their symptoms, and differences.
Table of Contents
The classification of adverse food reactions:
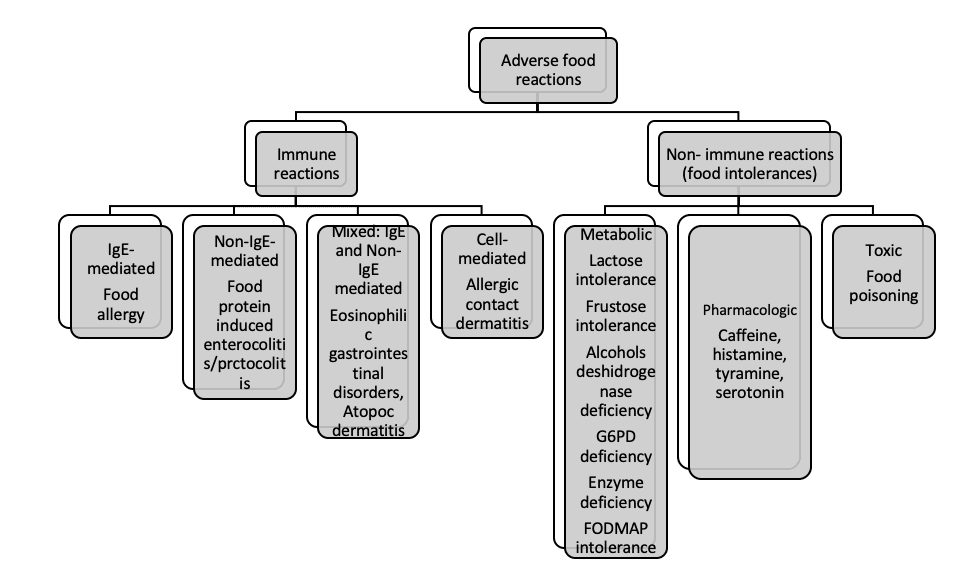
Non-immune adverse reactions:
These reactions include the toxic effect of food when it becomes spoiled and the patient’s metabolic reaction to food or medicine that their body cannot process.
Metabolic reactions:
The inability to metabolize or fully digest a certain food and therefore react adversely is what we know as food intolerance. Generally, food intolerances are related to a digestive enzyme deficiency followed by an inability to digest certain food, and commonly to the amount of food. Nevertheless, food intolerance is often confused by the patient with a food aversion, related to psychological distress caused when eating that food and provoking symptoms like nausea and vomiting.
- Food intolerance is a non-threatening, not an immune-mediated reaction.
- The most common gastrointestinal symptoms are:
- Gastrointestinal discomfort, bloating.
- Flatulence.
- Diarrhea
- Abdominal pain.
- Cramping
- Other symptoms may include:
- Headaches and migraines.
- Musculoskeletal problems.
- Behavioral changes.
Lactose intolerance:
Lactose is a sugar contained in food and its products; it is composed of galactose and glucose. Therefore it is a disaccharide. Later, when lactose enters our gut, the enzyme lactase separates lactose into galactose and glucose before its absorption. When lactase becomes unavailable, the indigestible lactose moves through the gut entering the bowel where bacterial fermentation begins. This, leading to gas production, and liquid gets drawn to the gut resulting in osmotic diarrhea.
The prevalence of lactose intolerance is varied among studies, reporting evidence from 7% to 20% in adults. It is believed that neonates have a functional amount of lactose, but this enzyme tends to decline after weaning.

Furthermore, the diagnose of lactose intolerance could be by made a food challenge test. In this test, the patient consumes 50g of a lactose load. Afterward, the symptoms related to the bloating and presence of osmotic diarrhea or flatulence confirm the diagnose. Likewise, the intensity of the symptoms is related to the type of product and the patient’s amount consumed. Needless to say, lactose intolerance is considered a variant of human metabolism rather than a disease.
Alcohol dehydrogenase deficiency:
In brief, alcohol dehydrogenase deficiency conduct to the inability to metabolize alcohol. Commonly found in patients of Asian descent. Flushing and vomiting are the most common symptoms of this kind of deficiency.
G6PD:
Glucose-6-phosphate dehydrogenase is a primary metabolic enzyme; its deficiency is caused by and a genetic disorder. This deficiency leads to oxidative injury to red blood cells due to the acute hemolysis caused by the ingestion of drugs or food.
Fructose intolerance:
In contrast with lactose, fructose is absorbed by diffusion in our gut with the help of a GLUT5 transporter and a glucose-dependent co-transporter, GLUT2. Hence, the fructose passive diffusion depends on a great matter of the concentration glucose. Accordingly, with lactose intolerance, the fructose’s remaining molecules enter the bowel, where colonic fermentation causes gas and inflammation.
Regularly, the gastrointestinal symptoms of enzyme deficiencies are related to the ones presented by patients with irritable bowel syndrome. Intolerances like lactose, alcohol, and fructose can be presented when the patient experiences changes in their microbiome or a viral infection. Therefore, medical diagnose could be easily misinterpreted.
Furthermore, in a descriptive study made in children, it was concluded that girls are more self-aware of symptoms related to food adverse reactions, and they tended to avoid more foods than their male counterparts. Interestingly, when symptom inducing foods were included in their diet, the symptoms were rarely related to severe symptoms caused by such foods’ ingestion. Lastly, the study supports the idea that children with IBS symptoms and self-perceived GI pain are more likely to have a decreased quality of life and psychological distress.
In conclusion, as a patient is essential to be aware of your symptoms and body. It is fundamental to know the differences of adverse reactions to food; the last information lets us have a higher quality of life and a better understanding of what is happening. Also, as a patient, it will improve the quality of diagnosing and prescription treatment. Lastly, you must know that each of these intolerances must be treated with a proper dietetic approach. The elimination of a specific group of food is likely to cause a nutritional deficiency.
Chumpitazi, Bruno P., et al. “Self-perceived food intolerances are common and associated with clinical severity in childhood irritable bowel syndrome.” Journal of the Academy of Nutrition and Dietetics 116.9 (2016): 1458-1464.
Yu, Linda Chia-Hui. “Intestinal epithelial barrier dysfunction in food hypersensitivity.” Journal of allergy 2012 (2012).
Turnbull, J. L., H. N. Adams, and D. A. Gorard. “The diagnosis and management of food allergy and food intolerances.” Alimentary pharmacology & therapeutics 41.1 (2015): 3-25.
Cox, Amanda L., and Scott H. Sicherer. “Classification of adverse food reactions.” Journal of Food Allergy 2.1 (2020): 3-6.
Disclaimers
Professional Scope of Practice *
The information herein on "Adverse Food Reactions" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's wellness blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-C) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on dralexjimenez.com, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card






