Explore how PRP injections for osteoarthritis can alleviate pain and improve joint function for those suffering from this condition.
Table of Contents
Abstract
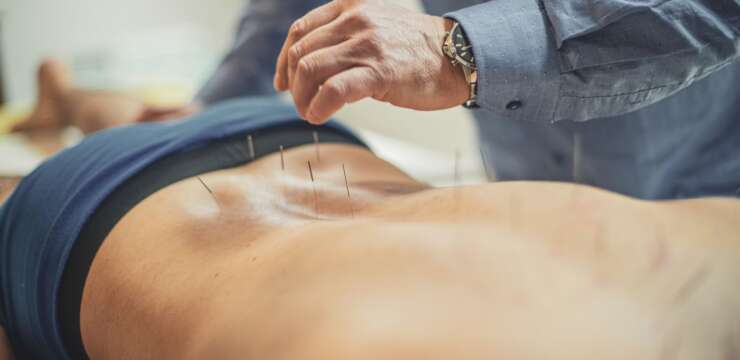
As Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, I guide you through the latest evidence on injection therapies for knee osteoarthritis (OA) and tendinopathy, comparing intra-articular corticosteroids, ketorolac, hyaluronic acid (HA), and platelet-rich plasma (PRP)—and explaining how dose and composition of PRP change outcomes at 6–12 months. I unpack the physiological mechanisms driving pain and disability in OA and tendinopathy and show how each injectate interacts with the synovium, cartilage, and periarticular tissues. You will find a clear, stepwise framework for choosing the right option for acute flares versus chronic symptoms, with practical pearls on patient selection, dosing strategy, risk mitigation, and surgical delay. Throughout, I show how chiropractic biomechanics, load management, targeted rehabilitation, metabolic optimization, and neuromuscular reeducation, when combined with injections, can multiply outcomes. I present recent findings from leading researchers (2017–2024), my clinical observations from Health Coach Clinic, and my professional updates, linking mechanisms to pragmatic care pathways that protect joint and tendon health.
Case-Based Introduction: Choosing the Right Injectate Under Real-World Pressure
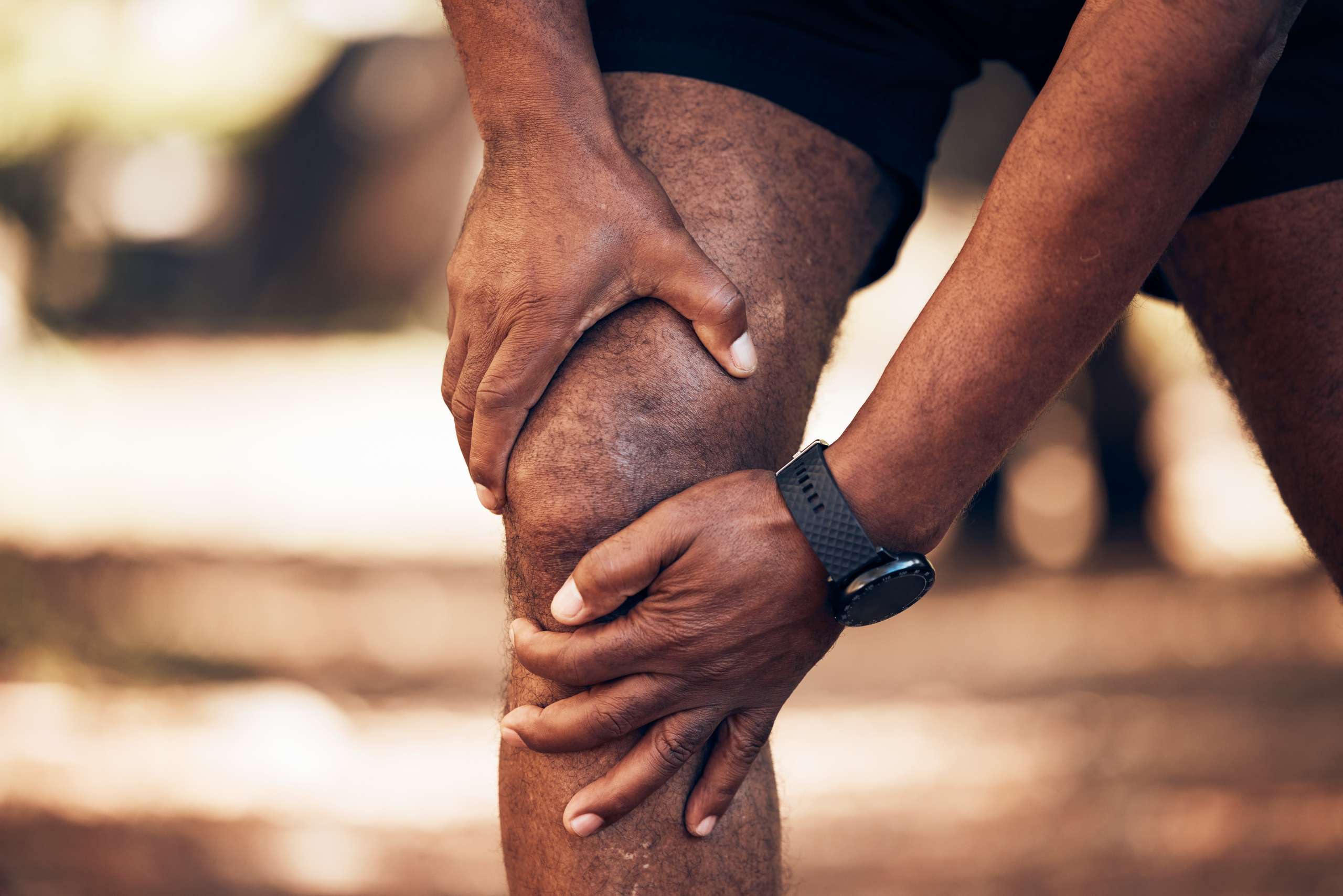
A story often reveals the decision-making we confront in the clinic. A 60-year-old woman with Kellgren-Lawrence grade 2 knee OA calls me on March 7, 2026—her son’s wedding is on March 14, 2026. She’s active, adherent to physical therapy, and has recently increased walking. Now she has a small effusion, medial joint line tenderness, and an antalgic gait. Radiographs confirm tricompartmental OA. She wants rapid relief.
Most clinicians reach for an intra-articular corticosteroid. But is that the best choice for short-term function, structural safety, and long-term outcomes? In this post, I synthesize the evidence so you can choose confidently—linking physiology to meaningful timelines and practical constraints.
Knee Osteoarthritis Pathophysiology: Why Synovial Inflammation Drives Pain
To select the right injectate, we must begin with the biology of OA pain:
- Synovial activation and effusion: Inflamed synovium releases IL-1?, TNF-?, and eicosanoids that sensitize nociceptors, increase joint fluid, and stretch the capsule—producing pain with movement and at rest.
- Cartilage catabolism: Upregulated matrix metalloproteinases (MMPs) and aggrecanases degrade proteoglycans and collagen, reducing cartilage’s ability to distribute load.
- Subchondral bone stress: Sclerosis and bone marrow lesions alter load transfer, fueling nociception and progression.
- Viscosupplement deficit: Endogenous hyaluronic acid falls in concentration and molecular weight, weakening lubrication and shock absorption.
- Peripheral and central sensitization: Repeated inflammatory signaling lowers joint pain thresholds and amplifies central pain processing.
Each injectate targets specific nodes in this network. Our job is to match mechanism to clinical need—balancing speed, durability, safety, and (when possible) disease modification.
Intra-Articular Corticosteroids: Rapid Synovial Quenching with Structural Caveats
When I deploy intra-articular corticosteroids, it’s to suppress synovial inflammation quickly:
- Mechanism: Steroids act via glucocorticoid receptors to suppress proinflammatory gene transcription, reduce leukocyte infiltration, and stabilize lysosomal membranes. This lowers effusion and provides prompt analgesia.
- Onset and duration: Relief typically begins within 3–7 days and wanes by 4–6 weeks (Systematic review and meta-analysis of intra-articular corticosteroids for knee osteoarthritis, 2024).
What the evidence shows:
- Short-term benefit: Meta-analytic data confirm meaningful short-term improvements in pain and function vs placebo (Systematic review and meta-analysis of intra-articular corticosteroids for knee osteoarthritis, 2024).
- Structural concern: A two-year RCT in JAMA found that triamcinolone, administered every 12 weeks, did not improve pain compared with saline and led to greater cartilage volume loss (McAlindon et al., 2017).
- Surgical signal: A large database analysis showed higher total knee arthroplasty (TKA) rates over five years among patients with prior steroid injections, with a dose-response relationship by frequency (Intra-articular corticosteroid injections and risk of knee arthroplasty, 2020).
Systemic considerations:
- Metabolic: Transient hyperglycemia, especially in diabetes, for up to a week.
- Bone health: Cumulative exposure raises concern for bone mineral density in postmenopausal women and men over 50.
- HPA axis: Potential adrenal suppression even after single exposures.
- Surgical timing: Many surgeons prefer a ~3-month interval between steroid injection and arthroplasty to mitigate the risk of infection.
My takeaway: For an acute flare with a hard deadline, steroids remain a tool—but I prefer safer, steroid-sparing options when possible to avoid chondrotoxicity and immunosuppression.
Ketorolac Intra-Articular Injection: Steroid-Sparing Rapid Analgesia
I increasingly use intra-articular ketorolac for fast relief without steroid-related risks:
- Mechanism: As a nonselective COX inhibitor, ketorolac reduces prostaglandin-mediated nociceptor sensitization and inflammation. Intra-articular delivery achieves high synovial concentrations with lower systemic exposure than oral NSAIDs.
- Onset and duration: Onset within days; effects can last weeks to a few months (Efficacy of intra-articular ketorolac in musculoskeletal conditions, 2023).
Evidence summary:
- Comparable relief: Systematic reviews show ketorolac provides pain and functional improvements similar to steroids from one week to three months, with minimal adverse events (Efficacy of intra-articular ketorolac in musculoskeletal conditions, 2023).
- Structural safety: Preclinical models have not demonstrated cartilage damage associated with repeated steroid use.
Contraindications:
- Avoid in peptic ulcer disease, advanced renal dysfunction, significant cardiovascular risk, bleeding disorders, or on anticoagulants—standard NSAID precautions apply.
My takeaway: For urgent, reliable analgesia without immunosuppression or cartilage risk, ketorolac is a strong, evidence-supported option.
Hyaluronic Acid Injections: Restoring Lubrication and Modulating Inflammation
I turn to hyaluronic acid (HA) for patients seeking medium-term relief and joint support:
- Mechanism: HA restores the viscoelasticity of synovial fluid, improving lubrication and shock absorption. Through CD44 receptor engagement on synoviocytes and chondrocytes, HA can downregulate MMPs, temper IL-1?, promote proteoglycan synthesis, and reduce nociceptor sensitivity.
- Molecular weight matters: High–molecular–weight HA appears more chondroprotective in basic science and may stimulate endogenous HA synthesis more effectively.
Evidence summary:
- Effect size and timeline: Analyses find a small but significant reduction in pain vs placebo, reaching ~90% of maximum by 1 month, peaking around 2 months, and persisting through 4–6 months (Viscosupplementation for knee osteoarthritis, 2023).
- Patient selection: Better response in individuals younger than 65 years, with a BMI > 25, with more severe baseline symptoms, and less severe radiographic changes.
- Surgical delay: Registry data suggest higher TKA-free survival at 1–2 years among HA recipients, especially with repeated courses, with lower median OA-related costs before TKA (Hyaluronic acid injections and delay to total knee arthroplasty, 2019).
Coverage varies:
- US guidelines are mixed (some downplay HA due to modest average effects), while several European societies support use. Insurance coverage can be inconsistent.
My takeaway: HA supports medium-term symptom control without immunosuppression and may modestly delay surgery. It is not a rapid flare solution but complements long-term strategies.
Platelet-Rich Plasma: Dose-Dependent Biologic with Signals of Disease Modification
The PRP conversation has matured: dose and composition—not just the label—drive outcomes.
Why PRP is different:
- Mechanisms: PRP concentrates autologous platelets and growth factors. It downregulates NF-?B inflammatory pathways, shifts macrophages from M1 to M2 phenotype, and promotes anabolic signals (VEGF, PDGF, TGF-?) that support chondrocytes, ECM maintenance, and subchondral microenvironment optimization.
- Preclinical signals: Animal models show reduced cartilage degeneration, thicker cartilage with improved matrix, reduced osteophyte formation, and decreased subchondral sclerosis.
Clinical evidence:
- Superiority to HA: A comprehensive meta-analysis (~1,900 patients) found PRP achieves greater symptom improvement than HA, with lower reintervention rates and higher odds of reaching MCID (Platelet-rich plasma vs hyaluronic acid for knee osteoarthritis, 2024).
- Delay to surgery: Retrospective survival analyses report substantial delays to TKA, with median delays exceeding five years among responders, and 85% avoiding TKA within five years (Effect of intra-articular platelet-rich plasma on time to total knee arthroplasty, 2021).
Formulation and protocol matter:
- Leukocyte-poor PRP (LP-PRP) is typically favored for intra-articular administration to limit protease-driven catabolism and reduce post-injection flares.
- Dosing: Many protocols favor 2–3 injections spaced 2–4 weeks apart, but dose calibration is critical.
PRP Dose Matters: Platelet Concentration and Total Delivered Platelets
Why does it change the outcome:
- Platelets carry alpha granule cargo—PDGF, TGF-?, IGF-1, VEGF, HGF, and IL-1Ra—that orchestrate repair, modulate inflammation, and guide matrix synthesis. Insufficient platelets blunt signals; excessive leukocytes can increase protease activity in joints.
- Dose-response meta-analytic trends suggest high-dose PRP yields stronger and more durable results, especially at 6–12 months.
Evidence synthesis:
- Studies with positive outcomes typically deliver around 5 billion total platelets, while “negative” studies hover near 2.2 billion.
- When stratified by total dose, >10 billion platelets across a treatment course outperform comparators at 6 months on WOMAC and maintain superiority at 12 months, with variability influenced by rehab adherence and psychosocial factors.
- Concentration targets commonly used for joints are 5–2.0 million platelets/?L of injectate; below ~1.0 million/?L, cartilage-directed benefits diminish.
Translating this to practice:
- A series of three injections at 5 mL each with 5–2.0 million/?L delivers about 22.5–30 billion platelets—consistent with high-dose regimens seen in successful cohorts.
- For tendinopathy, I often aim for ?3× baseline platelet concentration and consider LR-PRP to create a controlled early inflammatory stimulus that supports remodeling.
My clinical observation: Precise platelet dosing and structured rehab compliance are the two strongest predictors of durable success, aligning with the best current research trends I share on Health Coach Clinic and on my LinkedIn.
PRP Versus HA, Steroids, and Ketorolac: Choosing, Sequencing, and Combining
Mechanistic comparison:
- PRP: Dominates in chondroprotection, anti-inflammatory cytokine modulation, and matrix gene upregulation (e.g., COL2A1, ACAN, SOX9).
- HA: Superior in boundary lubrication, viscoelastic support, and CD44-mediated modulation; mild anti-inflammatory effects.
- Corticosteroids: Potent and short-lived anti-inflammatory activity; repeated exposure is catabolic to cartilage and tendon matrix.
- Ketorolac: COX inhibition yields analgesia and reduces prostaglandin-driven inflammation without steroid-like catabolism; effects are short- to medium-term.
When to combine PRP and HA:
- Select studies indicate PRP + HA can reduce synovial inflammatory markers (IL-1?, TNF-?, MMP-3, TIMP-1) more than PRP alone and extend clinical benefits toward 24 months in certain cohorts (Combined PRP and Hyaluronic Acid Reduces Synovial Inflammatory Markers and Improves Outcomes Compared with PRP Alone, 2021).
- In my practice, if HA is covered by insurance and mechanical symptoms dominate, I pair LP-PRP with mid–molecular-weight HA, timing sessions to maximize biological and mechanical effects while avoiding admixture in the same syringe.
Integrative Chiropractic Care: The Multiplier That Makes Biologics Work Harder
Biology responds to mechanics. To make PRP and other injectables “stick,” the joint and tendon must move well and be appropriately loaded. Here’s how I integrate chiropractic biomechanics and rehabilitation:
- Movement assessment: I analyze gait, foot/ankle mechanics, hip-knee-ankle alignment, and trunk/hip control. We correct aberrant valgus/varus stresses and torsional loads that perpetuate synovitis and cartilage stress.
- Manual therapy: Gentle joint mobilizations and soft-tissue work reduce capsular stiffness and improve arthrokinematics without provoking inflammation.
- Neuromuscular reeducation: Gluteus medius/maximus activation, quadriceps control (especially VMO), hip external rotation strength, and core stabilization center, patellofemoral, and tibiofemoral
- Progressive loading: Closed-chain drills, tempo-controlled eccentrics, isometrics, and later energy-storage exercises optimize tendon and cartilage mechanotransduction.
Why it works:
- Reduced shear and improved tracking enhance synovial fluid distribution, lower nociceptor drive, and diminish inflammatory cytokines.
- Tendons and cartilage are mechanoresponsive: appropriate loading engages integrins, FAK, mTOR, and MAPK signaling to support matrix synthesis—synergizing with PRP’s growth factors.
Timing with injectables:
- Ketorolac: Begin gentle mobility within 24–48 hours; escalate strengthening as pain subsides over 1–2 weeks.
- Steroid: Avoid aggressive overloading while analgesia is pronounced to prevent silent overuse; reassess weekly.
- HA: Emphasize low-impact conditioning during the peak (weeks 2–8); gradually advance strength.
- PRP: Relative rest for 48–72 hours; avoid NSAIDs for 7–10 days to preserve platelet signaling; begin graded loading at 1–2 weeks and advance through 6–12 weeks.
Tendinopathy Insights: Translating the Framework Beyond OA
Tendinopathy isn’t just inflammation—it’s a failed healing response:
- Pathobiology: Collagen disorganization, neovascularization, altered tenocyte signaling, and nociceptive neuropeptides drive pain. Peritendinous inflammation and bursitis may coexist.
- Injection choices:
- Avoid intratendinous steroids due to degeneration and rupture risk.
- Ketorolac can be considered for peritendinous flare analgesia when bursitis or peritendinous inflammation predominates.
- PRP supports matrix remodeling and modulates nociception in several tendinopathies (e.g., lateral epicondylopathy), with dose and leukocyte content tailored to tissue needs.
Rehabilitation cornerstone:
- Eccentric or heavy slow resistance training restores tendon capacity, gradually re-aligning collagen.
- Isometrics provide short-term analgesia; staged progressions regulate symptom-guided loading.
- Chiropractic integration: Correct thoracolumbar, pelvic, and foot/ankle contributors to tendon overload; craft return-to-sport plans aligned with tissue timelines.
My practice position:
- I avoid routine steroids around tendons. LR-PRP can be appropriate for chronic tendinopathy when paired with strict post-injection loading rules and neuromuscular re-education.
Practical Algorithms: Matching Mechanism to Patient Need
Acute OA flare with a hard deadline (e.g., March 14, 2026):
- Goal: Rapid pain relief, minimal downtime.
- Preferred option: Intra-articular ketorolac—onset within days, favorable cartilage safety, no immunosuppression.
- Alternative: If ketorolac is contraindicated, a cautious single low- to moderate-dose steroid with explicit risk discussion.
Chronic, recurrent OA symptoms:
- Goal: Durable relief, structural safety, potential disease modification.
- Preferred: LP-PRP dosed to deliver >10 billion total platelets across a short series; strongest evidence for sustained improvement over HA and steroid.
- Adjunct: High–molecular–weight HA for medium-term relief; consider sequencing PRP + HA to optimize mechanobiology when coverage allows.
Tendinopathy (e.g., lateral epicondylopathy):
- Regenerative first-line: High-dose PRP; consider LR-PRP for chronic cases.
- Loading strategy: Eccentrics and isometrics staged by soreness rules; integrate kinetic-chain corrections.
- Analgesia: Time-limited ketorolac if needed; avoid corticosteroids.
Metabolic and systemic optimization:
- Improve glycemic control, vitamin D, and body composition.
- Address sleep and stress to blunt central sensitization and improve healing signals.
Clinical Observations: What I See in Practice
From my integrative work at Health Coach Clinic and ongoing updates:
- High-dose LP-PRP in knee OA consistently improves WOMAC/KOOS at 6 months, with durability toward 12 months. Pairing with mid-weight HA can extend the benefit to 18–24 months in active patients who commit to neuromuscular retraining.
- For lateral epicondylopathy, LR-PRP plus staged eccentrics and isometrics outperforms passive care and shows lower recurrence at 12 months than steroid-centered pathways.
- Patients with prior steroid exposure can still benefit from PRP, though structural gains may be slower; adherence to progressive loading is critical.
- The clearest outcome drivers are precise platelet dosing and rigorous rehab compliance—both of which align with the literature I share publicly.
You can follow my case insights and protocols at Health Coach Clinic and my professional page:
Safety, NSAIDs, and Procedural Timing: Protecting the Biology
A frequent question is whether to combine ketorolac with PRP. I do not.
- NSAIDs can impair platelet activation and alter the inflammatory cascade required for regenerative effects; I advise avoiding NSAIDs before and shortly after PRP (Laudy et al., 2015).
- If ketorolac is used for a flare, I separate it temporally from PRP and screen for contraindications (renal function, GI risk, bleeding).
- I do not mix PRP with other injectables; I prefer sequenced strategies to preserve signaling clarity.
Why Mechanism-Guided Care Works
- Targeted biology: Steroids silence synovial gene expression; ketorolac blunts prostaglandin-driven nociception; HA restores biolubrication and modulates CD44; PRP orchestrates a balanced joint microenvironment with pro-resolving immune shifts.
- Tissue-specific timelines: Relief that arrives too fast can invite overuse; aligning rehab progression to biologic windows prevents setbacks.
- Systems thinking: Joints fail not just because of cartilage, but because of load distribution, neuromuscular control, metabolic stress, and sleep-driven healing capacity. Integrative care respects the whole system.
Conclusion: A Clear, Evidence-Based Path Forward
- Acute flares and imminent function needs: Choose intra-articular ketorolac when possible; reserve steroids for selected cases after frank discussion of risks and short duration.
- Chronic symptom control with structure-first thinking: Favor properly dosed LP-PRP for superior, durable relief and signals of disease modification; consider high–molecular–weight HA for additional medium-term support or in staged protocols.
- Integrative chiropractic care is the multiplier: Correct mechanics, manage load, optimize metabolism, and align rehab with biologic healing. This is how outcomes are maximized, and surgery can be delayed.
References
- Effect of Intra-articular Triamcinolone vs Saline on Knee Cartilage Volume and Pain in Osteoarthritis (McAlindon, T. E., et al., 2017). JAMA. doi.org/10.1001/jama.2017.8741
- Systematic review and meta-analysis of intra-articular corticosteroids for knee osteoarthritis (2024). Osteoarthritis and Cartilage.
- Intra-articular corticosteroid injections and risk of knee arthroplasty (2020). Osteoarthritis and Cartilage.
- Efficacy of intra-articular ketorolac in musculoskeletal conditions: A systematic review and meta-analysis (2023). Arthritis Care & Research.
- Viscosupplementation for knee osteoarthritis: a systematic review and meta-analysis of randomized trials (2023). British Journal of Sports Medicine.
- Hyaluronic acid injections and delay to total knee arthroplasty: A large database analysis (2019). Osteoarthritis and Cartilage.
- Platelet-rich plasma vs hyaluronic acid for knee osteoarthritis: a systematic review and meta-analysis of randomized controlled trials (2024). The Journal of Bone and Joint Surgery.
- Effect of intra-articular platelet-rich plasma on time to total knee arthroplasty: A retrospective survival analysis (2021). Osteoarthritis and Cartilage.
- Combined PRP and Hyaluronic Acid Reduces Synovial Inflammatory Markers and Improves Outcomes Compared with PRP Alone (2021). Arthroscopy.
- Platelet-rich plasma for musculoskeletal regeneration: outcomes and mechanisms (Andia, I., & Maffulli, N., 2018). International Orthopedics, 42(11), 2477–2488.
- The effectiveness of platelet-rich plasma in treating tendinopathy: a systematic review (Laudy, A. et al., 2015). British Journal of Sports Medicine, 49(14), 943–950.
SEO tags: knee osteoarthritis injections, intra-articular ketorolac, corticosteroid injection risks, hyaluronic acid knee OA, platelet-rich plasma knee OA, PRP dose optimization, leukocyte-poor PRP, PRP vs HA evidence, integrative chiropractic care, synovitis pain relief, CD44 hyaluronic acid, NF-kB PRP mechanism, knee pain flare management, tendinopathy PRP strategy, load management knee OA, chondrotoxicity steroids, delaying knee replacement, biomechanics neuromuscular reeducation, regenerative medicine chiropractic, WOMAC KOOS outcomes
Disclaimers
Professional Scope of Practice *
The information herein on "Osteoarthritis and Pain Relief Options Using PRP Injections" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's wellness blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-C) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on dralexjimenez.com, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card