Sciatica can range from mild to severe. Most individuals are familiar with severe cases because of the intense shooting throbbing pain. On the other hand, mild cases can present with little to no discomfort or pain but involve tingling, pins and needles, electrical buzzing, and numbing sensations. This can make individuals think there is nothing wrong and their foot just fell asleep. It can come from nowhere, as there was no obvious back or leg trauma causing injury. However, somewhere along the nerve’s path, the nerve has become compressed, pinched, trapped, stuck, or twisted, most likely from a spasming muscle group in the low back, buttocks, or legs causing the sciatica foot symptoms. Chiropractic, massage, and decompression therapy can relax the muscles, relieve the symptoms, release the nerve, and restore function.
Table of Contents
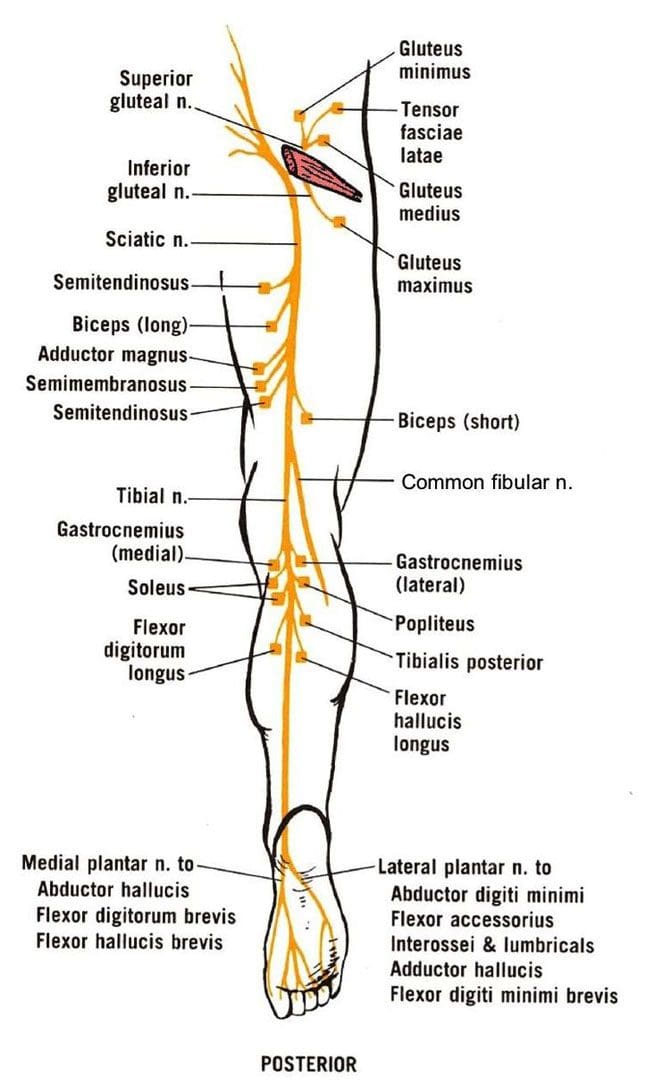
Sciatica Foot Symptoms
The sciatic nerve extends from the lower spine to the feet. Sciatica foot symptoms could be caused by several possibilities that range from piriformis syndrome to a developing slipped disc or spasming muscles. The symptoms travel through the nerve and can be felt anywhere along the nerve’s path, not necessarily at the source. This is why mild cases may only present with slight pricking/tingling sensations. However, left untreated, the cause can progress and develop into a severe case of sciatica.
Symptoms
The length of time that sciatica foot symptoms last will depend on the underlying cause. For example, if a herniated disc is the cause, the numbness may last for a few weeks or months until the disc heals. However, the numbness may be more long-lasting if sciatica is caused by degenerative disc disease. Sometimes, the nerve can be permanently damaged, leading to chronic pain and numbness. This is more likely to occur in individuals with diabetes or another condition that causes nerve damage.
- A varying degree of leg weakness can present as the spinal nerve root issues interfere with effective signal communication between the brain and the leg muscles.
- Leg weakness may also be interpreted as a pulling sensation in the leg.
- Weakness in the foot or toe muscles can also present.
- Leg movements such as walking, running, lifting the leg, or flexing the foot can also be affected.
- The tingling and numbing sensations may worsen when sitting or standing for long periods or moving the back in certain ways.
Treatment
Chiropractic care is an excellent option for treating sciatica foot symptoms and starts with a personalized plan based on individual symptoms, injury, and medical history. Chiropractors are neuromusculoskeletal experts on the spine, vertebrae, surrounding muscles, tissues, and nerves. Treatment includes spinal and extremity adjustments to realign the body, decrease inflammation, relieve pressure, release the nerve, and ultimately allow the body to activate its natural healing processes.
Massage
- Massage therapy can relieve muscle tension and spasms in the back and legs, reducing pressure on the sciatic nerve.
- Massage also increases blood circulation and relaxes the muscles, speeding healing and recovery.
Electrical Stimulation
- Electrical stimulation activates the nerves and muscles and reduces symptoms by blocking signals.
Physical Therapy
- Physical therapy exercises can help stretch and strengthen the back and leg muscles.
- Targeted exercises can be done at home to continue strengthening and maintaining the muscles.
Foot Orthotics
- Using orthotic devices such as arch supports or heel cups can help relieve pressure on the feet.
- Arch supports are especially helpful if sciatica foot symptoms are exacerbated by flat feet or other foot conditions.
- Heel cups can help with the frequent use of high heels.
Sciatica Specialists
References
American Academy of Orthopaedic Surgeons. “Sciatica.” orthoinfo.org/en/diseases–conditions/sciatica/
Cleveland Clinic. “Sciatica.” my.clevelandclinic.org/health/diseases/12792-sciatica#management-and-treatment
Emary, Peter C. “Evidence-based prognostication in a case of sciatica.” The Journal of the Canadian Chiropractic Association vol. 59,1 (2015): 24-9.
Frost, Lydia R et al. “Deficits in foot skin sensation are related to alterations in balance control in chronic low back patients experiencing clinical signs of lumbar nerve root impingement.” Gait & posture vol. 41,4 (2015): 923-8. doi:10.1016/j.gaitpost.2015.03.345
Mayo Clinic. “Sciatica.” www.mayoclinic.org/diseases-conditions/sciatica/symptoms-causes/syc-20377435?p=1
National Institutes of Health. “Sciatica.” medlineplus.gov/sciatica.html
Shakeel, Muhammad, et al. “An uncommon cause of sciatica.” Journal of the College of Physicians and Surgeons–Pakistan: JCPSP vol. 19,2 (2009): 127-9.
Tampin, Brigitte, et al. “Disentangling ‘sciatica’ to understand and characterize somatosensory profiles and potential pain mechanisms.” Scandinavian journal of pain vol. 22,1 48-58. 2 Aug. 2021, doi:10.1515/sjpain-2021-0058
Disclaimers
Professional Scope of Practice *
The information herein on "Sciatica Foot Symptoms: EP Health Coach Clinic" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's wellness blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-C) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on dralexjimenez.com, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card