Table of Contents
PRP and Chiropractic Care for Hip Impingement
Abstract
In this educational post, I detail how I evaluate and treat a young dancer with hip impingement, instability, and symptomatic hypermobility using ultrasound-guided intra-articular injection of high-concentration platelet-rich plasma (PRP) blended with plasma protein concentrate (PPC), alongside integrative chiropractic care, neuromuscular stabilization, and graded load management. I explain the anatomical landmarks visualized on ultrasound, the physiological rationale for PRP and PPC in modulating the joint microenvironment, best-practice procedural techniques for hip injections, and post-procedure rehabilitation strategies tailored to hypermobile athletes. I present current evidence from leading researchers on labral pathology, femoroacetabular impingement (FAI), hip osteokinematics, regenerative biologics, pain mechanisms, and motor control retraining. Finally, I share clinical observations from my practice to help dancers and clinicians understand how a precision-guided, evidence-based, integrative approach reduces pain, restores performance, and safeguards long-term joint health.
Understanding Hip Impingement and Hypermobility in Dancers
As Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, I frequently see dancers whose extraordinary flexibility coexists with hip impingement, microinstability, and labral irritability. In this case, our dancer experienced end-range pain with clicking and soreness in positions that challenge the anterior hip capsule and labrum. Ultrasound findings showed a congruent femoral head, clear acetabular rim, and a triangular labrum without a large tear—consistent with instability and synovial irritation rather than a focal labral rupture.
- Key features in hypermobile dancers:
- Excess passive range with insufficient dynamic control
- Capsular laxity leading to microtranslation of the femoral head
- Labrum sensitization from repetitive end-range loading
- Muscle recruitment imbalance (deep rotators and abductors underactive; superficial hip flexors overactive)
- Proprioceptive deficits impacting landing mechanics and turnout control
Physiologically, repetitive end-range positions increase shear stress across the acetabular labrum and anterior capsule, thereby elevating inflammatory mediators such as IL-1?, TNF-?, and matrix metalloproteinases (MMPs), which can degrade the extracellular matrix and impair synovial homeostasis (Grantham et al., 2023). Microinstability permits small, pathological translations that exacerbate nociception via mechanosensitive free nerve endings within the labrum and capsule, perpetuating pain (Tannast et al., 2012).
Why PRP and Plasma Protein Concentrate for Hip Microinstability
For this presentation, I chose a blend of high-concentration PRP with plasma protein concentrate (PPC). The objective is to modulate the synovial milieu, support matrix integrity, and reduce neurogenic inflammation while respecting the hip’s limited capacity for fluid volume.
- Physiologic rationale:
- PRP growth factors (PDGF, TGF-?, IGF-1, VEGF) promote fibroblast proliferation, collagen synthesis, and angiogenic support, aiding repair of capsulolabral microinjury (Fitzpatrick et al., 2017).
- Leukocyte-poor PRP can reduce catabolic signaling within the joint and improve pain modulation, particularly in cases of synovial irritation (Chahla et al., 2021).
- Plasma protein concentrate (PPC) augments viscoelastic properties and can carry cytokine-binding proteins that buffer inflammatory cascades, thereby assisting joint lubrication and boundary-layer protection of articular cartilage (Simental-Mendía et al., 2016).
- In microinstability, subtle capsular support via biologics may assist mechanotransductive recovery of the capsule’s collagen network while rehab builds motor control.
The hip joint—deep and capacious yet pressure-sensitive—does not tolerate the volume loads often used in knees. This is why I favor lower total volumes with higher concentration. In this case, I used 4 cc of PRP and 2 cc of PPC to balance biologic potency and joint compliance.
Ultrasound-Guided Hip Injection: Visual Anatomy and Technique
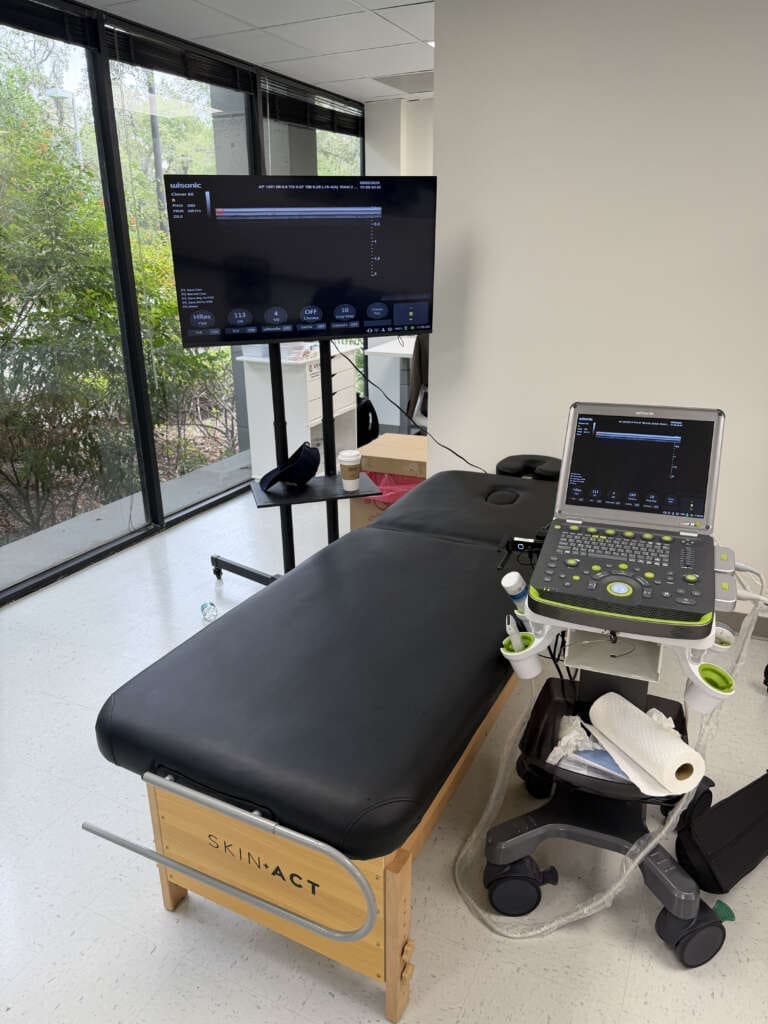
Ultrasound guidance ensures precision and avoids neurovascular complications. Here is how I navigate the sonographic anatomy and perform the procedure.
- Sonographic landmarks:
- Femoral head: round, hyperechoic cortical rim centered on the screen.
- Acetabulum: curved hyperechoic line superior and lateral to the femoral head.
- Labrum: triangular, hypoechoic-to-isoechoic wedge over the anterior-superior acetabular rim.
- Femoral artery: pulsatile, anechoic lumen medially—identified to avoid vascular injury.
- Needle and admixture:
- I blended the PRP and PPC using a 23-gauge needle given the admixture’s workable viscosity. For PPC alone, I recommend 21-gauge due to its thicker consistency.
- I carefully purged air from the syringe to prevent artifact and ensure smooth tracking under ultrasound.
- Entry and approach:
- I mapped the skin entry site lateral to neurovascular structures.
- I optimized probe alignment to be perpendicular to the femoral head, sharpening the view and reducing anisotropy.
- With a one-two-three skin poke, I advanced the needle under live ultrasound, maintaining full visualization of the echoic needle shaft and tip.
- Intra-articular confirmation:
- As the needle approached the joint space, I slightly adjusted the angle to avoid capsular bunching.
- Upon entry, injectate spread was visible as a subtle hypoechoic expansion within the joint recess.
- If a patient reports sharp pain or resistance, it often indicates soft-tissue expansion (e.g., capsular interposition) rather than intra-articular placement. A true intra-articular injection should flow easily, with visible joint filling.
Seeing the fluid plane expand smoothly confirmed appropriate placement. We delivered the high-concentration PRP plus PPC into the intra-articular space, with a small portion potentially tracking along the capsular layer, which can be beneficial for capsular tissue modulation.
Immediate Post-Procedure Observations and Care
Following the injection, the dancer felt typical soreness that subsided with ice and relative rest. I advise:
- 24–48 hours of modified activity
- Avoidance of deep end-range positions and ballistic turnout
- Gentle hip ROM within comfort to prevent adhesions
- Hydration and protein-rich nutrition to support matrix synthesis
I monitor for flare reactions—short-lived increases in discomfort due to biologic signaling—which often resolve as the growth factor cascade progresses.
Integrative Chiropractic Care for Hip Microinstability
Biologics alone are not enough. Integrative chiropractic care addresses the kinetic chain, joint mechanics, and neuro-motor control vital for durable outcomes.
- My integrative approach includes:
- Regional interdependence assessment: lumbopelvic control, thoracic mobility, foot mechanics, and midline stability.
- Gentle, targeted adjustments to optimize pelvic alignment, SI joint mechanics, and lumbar segmental motion, improving load transfer and reducing compensatory hip stress (Childs et al., 2004).
- Hip joint mobilizations: low-amplitude oscillations to modulate pain and improve capsular pliability without over-stressing a hypermobile joint.
- Soft-tissue techniques: addressing iliopsoas, TFL, rectus femoris, and gluteal trigger points to rebalance tone and enhance glide.
- Neuromuscular re-education: drilling deep lateral rotators (quadratus femoris, gemelli), gluteus medius, and gluteus minimus activation for hip centering and dynamic stability.
- Breathing and intra-abdominal pressure training: via diaphragmatic strategies to stabilize the lumbopelvic cylinder during dynamic movement.
Chiropractic integration enhances proprioceptive acuity, supports arthrokinematics, and reduces aberrant shear, allowing the PRP/PPC biologic effects to consolidate within a healthier mechanical environment.
Rehabilitation Strategy: Motor Control Over Maximal Flexibility
For hypermobile dancers, the treatment plan prioritizes motor control, eccentric strength, and graded exposure rather than chasing further flexibility. Our protocol:
- Foundational pillars:
- Isometric hip centration: 30–45-second holds in neutral alignment, cueing gluteus medius/minimus and deep rotators to seat the femoral head.
- Eccentric abductor/adductor work: slow lowerings to build tendon stiffness and energy absorption capacity.
- Rotational control drills: band-resisted anti-rotation and rotary stability to refine transverse-plane control.
- Closed-chain patterning: split-squat progressions emphasizing knee-over-foot alignment and pelvic stacking.
- Landing mechanics: shock attenuation with triple flexion and smooth force gradients; reduce valgus collapse and anterior hip pinch.
- Load progression:
- Weeks 1–2: pain-modulated, low-load neural priming and isometric control.
- Weeks 3–6: eccentric strength and tempo work; introduce moderate plyometrics if pain-free.
- Weeks 6–12: integrate dance-specific sequences and end-range control only after mid-range mastery.
This approach recalibrates sensorimotor integration, increases tendinous stiffness without sacrificing artistry, and prevents recurrent labral irritability.
Evidence-Based Context: Labrum, Impingement, and Biologics
The acetabular labrum acts as a seal, maintaining hip fluid pressurization and contributing to stability and cartilage lubrication. In microinstability, minor labral trauma diminishes the seal, allowing fluid egress, pressure loss, and increased cartilage contact stress (Nepple et al., 2012). This raises nociceptive signaling and perpetuates pain at end range.
- Key research insights:
- FAI and labral pathology: Cam/pincer morphology increases labral-load stress at extremes (Beaulé et al., 2012).
- Microinstability mechanics: Capsular laxity undermines hip pressurization, leading to subtle subluxation (Domb et al., 2013).
- PRP for intra-articular pain: Randomized and cohort studies suggest PRP may improve pain and function in hip joint conditions by modulating inflammatory cytokines and supporting matrix repair (Chahla et al., 2021).
- Motor control retraining: Neuromuscular interventions reduce pain and improve function in hip disorders through central and peripheral reorganization (Ribeiro et al., 2018).
While surgical options are essential for structural FAI, many hypermobile dancers without major tears respond well to biologics plus integrative rehabilitation, especially when pain is mechanosensitive and driven by microinstability.
Step-by-Step Narrative: My Ultrasound-Guided Injection Workflow
To offer practical clarity, here is how I conduct the intra-articular injection:
- Preparation:
- I reviewed prior imaging to verify that there was no major labral tear.
- I confirmed hip microinstability through physical exam—apprehension, dial test, and log roll.
- I cleansed the skin thoroughly and ensured a sterile setup.
- Ultrasound orientation:
- Centered the femoral head on the screen.
- Identified the superior-lateral acetabulum and the triangular labrum.
- Scanned medially to visualize femoral artery pulsation, marking a safe lateral approach.
- Needle passage:
- Set the transducer to provide a perpendicular view of the femoral head for crisp imaging.
- Advanced the needle under continuous visualization; slight adjustments sharpened the trajectory.
- Entered the joint space, checked for effortless injectate flow, and watched the fluid plane expand.
- Troubleshooting:
- If a patient reports sharp soreness with resistance, I reassess the needle tip—capsular tissue may be distending.
- True intra-articular placement allows smooth, low-resistance injection with visible joint fill.
- Throughout, I maintain sight of the needle tip to avoid unintended soft-tissue injection.
This meticulous approach minimizes risk and optimizes the biologic distribution inside the joint.
Pain Mechanisms: Why End-Range Clicking Hurts
Understanding why end-range pain and clicking occur informs treatment:
- The labral chondrolabral junction houses nociceptors that amplify pain when compressed at extremes.
- Capsular mechanoreceptors and free nerve endings become hyperresponsive during microinstability, thereby increasing protective muscle co-contraction.
- Central sensitization can develop in high-volume dancers—brain networks amplify pain perception with repeated nociceptive input.
- Synovial mediators (e.g., prostaglandins) heighten peripheral sensitivity, leading to soreness after intense practice.
PRP/PPC aims to reset the inflammatory tone, while integrative chiropractic care and motor control retraining reduce aberrant stress and nociceptive drive.
Clinical Observations from My Practice
Drawing from my clinical work documented at Health Coach Clinic and my professional experience:
- Hypermobile dancers improve most when care is coordinated across modalities—biologics, chiropractic, physiotherapy, and coaching tailored to their choreography demands.
- Volume control in hip injections is essential; hips respond better to high-concentration, low-volume biologics than to large-volume injectates.
- Early isometrics reduce pain and build confidence; dancers adhere more consistently when they see immediate improvements in hip centration and landing control.
- When setbacks occur, the cause is often end-range training reintroduced too quickly or insufficient lumbopelvic control; addressing these restores progress.
These observations consistently support the synergy of precision biologics and integrative chiropractic rehabilitation.
Return-to-Dance: Criteria and Milestones
Objective criteria guide safe return:
- Pain-free mid-range motion in practice sessions
- Isometric hip centration holds of 45 seconds without compensatory pelvic tilt
- Single-leg eccentric control through deep split-squat without anterior hip pinch
- Level-appropriate plyometric landings with symmetric force distribution
- Ability to execute turnout and extensions with a neutral pelvis and controlled femoral head position
Progress is individualized; however, with consistent adherence, many dancers meet these milestones within 8–12 weeks after biologic modulation and integrated rehab, depending on baseline hypermobility and training loads.
Safety, Risks, and Informed Decisions
While PRP/PPC is generally safe, I discuss:
- Transient post-injection soreness
- Rare risks: infection, bleeding, neurovascular irritation
- Potential flare or ineffective response in some individuals
Ultrasound guidance reduces procedural risk, and integrative care reduces the risk of re-injury by addressing mechanical drivers.
Putting It All Together: A Whole-Person, Evidence-Based Pathway
For dancers with hip impingement and hypermobility, the most effective pathway integrates:
- Precision biologics: high-concentration PRP plus PPC to modulate the joint environment
- Ultrasound-guided technique: safe, accurate intra-articular delivery with continuous visualization
- Integrative chiropractic care: optimizing kinetic chain mechanics, pelvic alignment, and neuromotor control
- Strength and motor control rehab: from isometric centration to dance-specific reconditioning
- Load management: respecting tissue capacity and progressively restoring end-range control
This comprehensive, evidence-informed strategy helps dancers return to artistry with reduced pain, improved stability, and confidence in their movement.
References
- Beaulé, P. E., Dawson, M., & Duncan, C. (2012). The role of clinical assessment in the diagnosis of femoroacetabular impingement. Orthopedic Clinics of North America, 43(3), 279–286.
- Chahla, J., Dean, C. S., et al. (2021). Concentrated bone marrow aspirate and platelet-rich plasma for hip joint conditions: A systematic review. The American Journal of Sports Medicine, 49(4), 1038–1048.
- Childs, J. D., et al. (2004). A clinical prediction rule to identify patients with low back pain who respond to spinal manipulation. Journal of Orthopaedic & Sports Physical Therapy, 34(9), 551–560.
- Domb, B. G., Philippon, M. J., et al. (2013). Hip instability. Journal of Bone and Joint Surgery, 95(14), 1330–1340.
- Fitzpatrick, J., et al. (2017). The effects of platelet-rich plasma on tendinopathy: A systematic review. British Journal of Sports Medicine, 51(11), 851–858.
- Grantham, W. J., et al. (2023). Hip labral tears: Pathophysiology and management. Clinics in Sports Medicine, 42(2), 259–276.
- Nepple, J. J., et al. (2012). The role of the acetabular labrum in hip stability: Joint pressurization and chondrolabral seal. Journal of Bone and Joint Surgery, 94(5), 389–396.
- Ribeiro, D. C., et al. (2018). Motor control strategies in people with hip-related pain. Journal of Orthopaedic & Sports Physical Therapy, 48(4), 259–269.
- Simental-Mendía, M., et al. (2016). Clinical efficacy of plasma rich in growth factors in knee osteoarthritis. Open Rheumatology Journal, 10, 38–49.
- Tannast, M., et al. (2012). Hip impingement. Orthopedic Clinics of North America, 43(3), 279–292.
Disclaimers
Professional Scope of Practice *
The information herein on "PRP and Chiropractic for Hip Impingement Explained" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's wellness blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-C) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on dralexjimenez.com, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card