Table of Contents
Introduction
The gut and the brain have two different jobs that do different functions in the body but, have a bidirectional communication with each other. The brain is part of the central nervous system that sends out neuron signals all throughout the entire body. These neuron signals make sure that everything is working properly, from the heart beating to blood pressure being regulated. The gut is part of the digestive system and it makes sure that food is being digested properly, while the beneficial good bacteria is protecting the gut from harmful pathogens. When unwanted pathogens start to affect either the brain, the gut, or both, it can cause problems to the body making it dysfunctional and causing the individual unwanted pain. In this 2 part series, we will be taking a look at the different factors that can affect the gut-brain axis. Part 1 took a look at what the gut-brain axis is and how does it function in the body. By referring patients to qualified and skilled providers who specialized in gastroenterology services. To that end, and when appropriate, we advise our patients to refer to our associated medical providers based on their examination. We find that education is the key to asking valuable questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, in case you are uncertain here is the link to all the insurance providers we cover. If you have any questions, please call Dr. Jimenez at 915-850-0900.
The Gut-Brain Connection
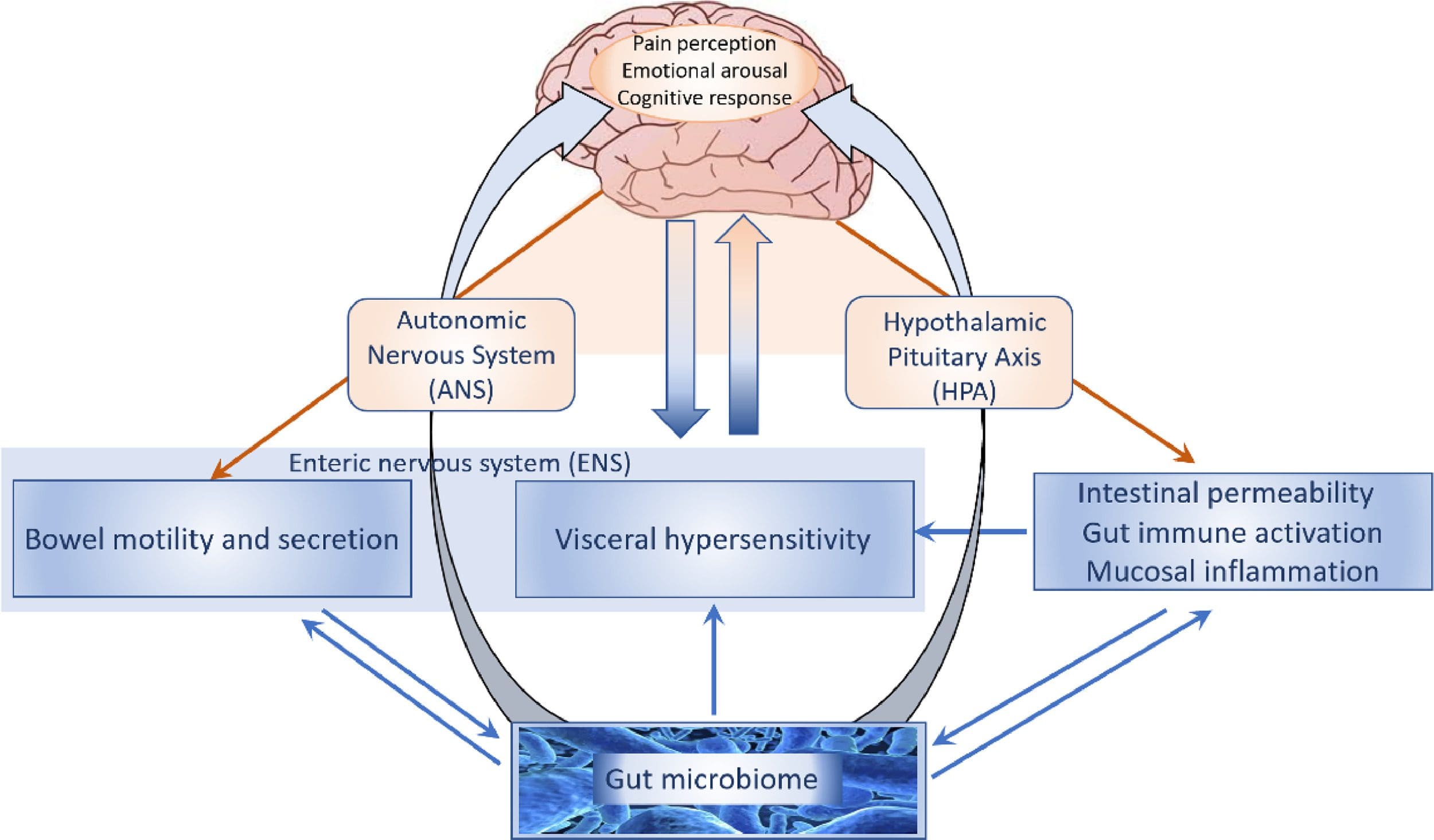
The gut-brain connection provides a bidirectional connection to both the brain and the gut. Both of these organs continuously send each other signals back and forth in order to make sure that the body is functioning properly while also doing their jobs as well. Research studies show that the gut-brain connection is also known as the enteric nervous system and what it does is that it’s a network of nerves, neurons, and neurotransmitters that extends all over the entire digestive tract. The enteric nervous system is also referred to as a “second brain”, which is the gut as it is in constant communication to the brain and plays a major key role in diseases and mental health for individuals.
HCTP Therapy
Stem cells* or HCTP (human cellular tissue products) are a form of regenerative cellular treatments that help boost the body’s own natural healing process. HCTP has been used in both international and nationally affiliated clinics and distribution organizations by repairing and regenerating damaged cells, diseased tissues, and organs back to their original state and function in the body. With more upcoming research about the beneficial properties of HCTP, many individuals can get their lives back together pain-free and without chronic issues affecting them.
The Factors That Affect The Gut-Brain
There are many factors that can affect both the gut and the brain as the body does encounter many pathogens that can cause a person to be in pain. Studies have found that gut microbiota has been known to support tight junction integrity and when dysbiosis and increased intestinal permeability can cause dysfunction to the brain. The same goes for the brain when the neuron signals are being disrupted by unwanted pathogens that travel from the brain to the gut. Other factors that can affect the gut-brain axis include:
- Sedentary lifestyle
- Unhealthy diet
- Physical inactivity
- Stress
- Inflammation
- Chronic pain
Visceral Pain
Research shows that visceral pain is described as pain originating from the internal organs of the body and can cause the development of neurological behavioral disorders. Visceral pain can also cause gastrointestinal disorders as it causes damage to the thorax and abdomen while also making maladaptive changes to alter the brain structure and function. Other research studies have found that visceral pain is a complex and heterogeneous disorder that involves the spinal cord, a higher order of the brain structure, and manipulates the gut microbiota. Some of the mechanical features that visceral pain causes gastrointestinal pain and discomfort that can cause painful stimuli to the brain.
Stress
Stress can be both beneficial and harmful to the body, especially to the gut and the brain. When stress is in its acute form, it can help give the body a “fight or flight response” effect that gives the body a little boost of energy. However, when stress is in its chronic state can cause damage to the brain and gut as it can become harmful over time if it is not treated. Studies show that the importance of the gut-brain axis in regulating stress responses has been long appreciated as it can impact mental and gut health. When stress starts to affect both the gut and the brain, the neuron signals will get disrupted and can kill the neuron’s signals and replaced them with new ones to cause havoc on the gut-brain axis. Other studies have found that when a person is under chronic stress, gut infections and inflammation can cause an increase in high-co-morbidity of anxiety and depression disorders in people.
Inflammation
Just like stress, inflammation can be both beneficial and harmful to the body and the brain-gut connection. The beneficial factor of inflammation in its acute form is that it can naturally heal an injury by making the affected area swell up, red, and hot to the touch which can last for a few minutes to an hour, depending on the injury. Studies have shown that the gut-brain connection has molecular and cellular mechanisms that regulate inflammatory responses to the body. However, just like chronic stress, when the body has chronic inflammation can cause havoc on the gut by attaching itself to the intestinal permeability and causing the immune system to attack the permeability causing a leaky gut. For the brain, inflammation can attach to the neuron signals and travel up to the brain to cause havoc on the blood-brain barrier and develop neuroinflammation.
Conclusion
All in all, the gut-brain connection has a wonderful bidirectional connection that makes sure that not only the body is staying functional, but also for each of the organs to do their jobs properly as well. When unwanted pathogens start to affect the brain-gut connection, it can cause numerous problems to the body with chronic inflammation, chronic stress, and many other issues that can cause a person to be in pain. Utilizing a healthy diet filled with nutritional food, getting up to do some sort of physical exercise, and making small changes to a lifestyle habit can dampen the effects of chronic issues that are affecting the body and provide the individual with a pain-free lifestyle.
References
Agirman, Gullistan, et al. “Signaling Inflammation across the Gut-Brain Axis.†Science (New York, N.Y.), U.S. National Library of Medicine, 25 Nov. 2021, pubmed.ncbi.nlm.nih.gov/34822299/.
Appleton, Jeremy. “The Gut-Brain Axis: Influence of Microbiota on Mood and Mental Health.†Integrative Medicine (Encinitas, Calif.), InnoVision Health Media Inc., Aug. 2018, www.ncbi.nlm.nih.gov/pmc/articles/PMC6469458/.
Bear, Tracey, et al. “The Microbiome-Gut-Brain Axis and Resilience to Developing Anxiety or Depression under Stress.†Microorganisms, MDPI, 31 Mar. 2021, www.ncbi.nlm.nih.gov/pmc/articles/PMC8065970/.
Foster, Jane A, et al. “Stress & the Gut-Brain Axis: Regulation by the Microbiome.†Neurobiology of Stress, U.S. National Library of Medicine, 19 Mar. 2017, pubmed.ncbi.nlm.nih.gov/29276734/.
Medical Professionals, Cleveland Clinic. “Gut-Brain Connection: What It Is, Behavioral Treatments.†Cleveland Clinic, 3 Dec. 2020, my.clevelandclinic.org/health/treatments/16358-gut-brain-connection.
Moloney, Rachel D, et al. “Stress and the Microbiota-Gut-Brain Axis in Visceral Pain: Relevance to Irritable Bowel Syndrome.†CNS Neuroscience & Therapeutics, John Wiley and Sons Inc., Feb. 2016, www.ncbi.nlm.nih.gov/pmc/articles/PMC6492884/.
Pusceddu, Matteo M, and Melanie G Gareau. “Visceral Pain: Gut Microbiota, a New Hope? – Journal of Biomedical Science.†BioMed Central, BioMed Central, 11 Oct. 2018, jbiomedsci.biomedcentral.com/articles/10.1186/s12929-018-0476-7.
Disclaimer
Disclaimers
Professional Scope of Practice *
The information herein on "An Overview On Different Factors Affecting Gut-Brain Axis | Part 2" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's wellness blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-C) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on dralexjimenez.com, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card