Table of Contents
Introduction
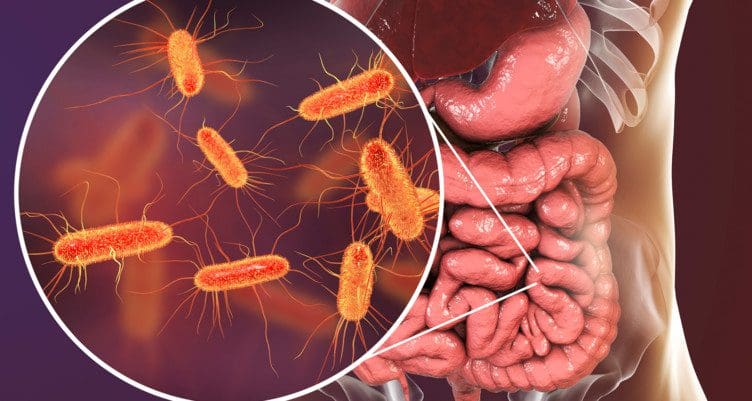
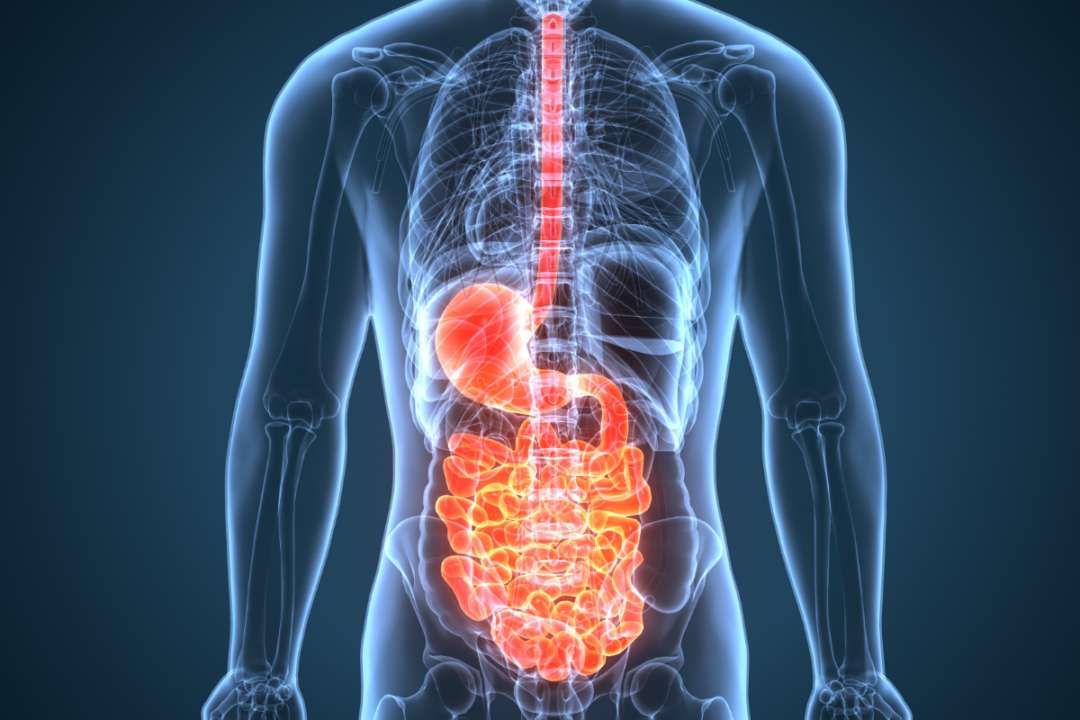
The gut system is home to many beneficial bacteria that ensure that everything is working correctly. The organs that make up the gut system help transport the nutrients and oxygenated blood to the muscles, tissues, vessels, and nerve roots that allow the body to function. The gut also communicates with the brain and the immune system to provide the necessary energy to make the body move from one place to another. When disruptive factors start to mess with the gut microbiota, it can cause inflammatory factors and other gut-related issues to wreck the intestinal walls of the gut and affect the overall health of a person. Today’s article post will focus on the gut microbiome’s role in the body, the metabolic functioning of gut bacteria, and how different factors can affect the gut from functioning correctly. Referring patients to qualified and skilled providers who specialize in gastroenterology treatments. We guide our patients by referring to our associated medical providers based on their examination when it’s appropriate. We find that education is essential for asking insightful questions to our providers. Dr. Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, it may. If you are uncertain, here is the link to all the insurance providers we cover. If you have any questions or concerns, please call Dr. Jimenez at 915-850-0900.
The Gut Microbiome’s Role In The Body
Have you been feeling sick to your stomach? Do you feel bloated around the mid-section of your body? Have you been feeling sensitive to the food you have been consuming? Many of these symptoms are gut-related issues that affect the gut microbiome. The gut microbiota plays a critical metabolic role in many systems that help keep the body functional by maintaining delicate balance and cross-talking with the immune system. Research studies have shown that the gut microbiome is homed to a very complex and dynamic population of gut flora that influences the body. Since the gut microbial ecosystem is considered the largest endocrine organ in the body, it can produce various biologically active compounds that are the same as hormones. These compounds are carried in circulation and distributed to distant sections within the host, influencing different essential biological processes. Other research studies have mentioned that the intestinal tract in the body has an integrated resilient ecosystem that can be influenced by the many factors that affect the gut microbiome in its composition and changes. Some of these changes benefit good bacterial growth in the gut microbiota.
The Metabolic Function Of Gut Bacteria
When a person consumes nutritional foods, it travels into the gut to be biotransformed into nutrients. It makes its way into the intestines, where it is stored and ready to be distributed to the rest of the body. When digestive food is sitting in the intestines, that is where the beneficial gut bacteria comes in and helps shape the gut microbiota. Research studies have shown that the beneficial bacteria in the intestines play a critical role in the gut microbiome as it helps maintain immune and metabolic homeostasis. The gut bacteria’s metabolic function to the body helps break down dietary fibers that then get turned into SCFAs (short-chained fatty acids). Other tasks that gut bacteria do for the gut microbiome include:
- Production of Phenols
- Breakdown of oligosaccharides
- Helps regulate Fats, TG, and Cholesterol
- Vitamin absorption
- Mucous production
- Detoxification
An Overview Of a Diverse Gut-Video
Have you been feeling sluggish throughout the entire day? Do you feel constipated or bloated? Have you become sensitive to your favorite foods? If you have been experiencing these issues throughout your whole life, it could be due to your gut microbiome talking to you. The video above explains how the gut microbiome is one of the essential organs in the body since it helps with biodiversity in the gut system. The importance of greater microbial diversity is associated with the body’s ability to deal with stressors, such as opportunistic pathogens or dietary perturbations affecting the digestive system. When individuals have gut-related diseases, they are more likely to alter their gut microbiome than healthy individuals. Multiple associations between reduced microbial diversity and illness are recorded in the literature for people to find out what is going on in their gut system. Keeping a healthy gut can prevent risk factors like metabolic diseases such as type 2 diabetes, IBD (inflammatory bowel disease), SIBO, and other gut risk factors from affecting the gut.
Factors That Can Affect The Gut
When there is a state of imbalanced microbial ecology that contributes to affecting the gut bacteria ratio, it can cause many chronic diseases that cause the body to be dysfunctional. The overgrowth of micro-organisms in low intrinsic virulence induces disease by altering:
- The nutritional status
- The immune response
- The elimination capacity of the host
Research studies have found that factors affecting the gut microbiome can trigger the inflammatory pathways attacking the gut intestinal walls and letting the bacteria leak out. Other factors like stress or emotional outburst can cause the growth of harmful bacteria to overpopulate the good bacteria. This causes the gut microbiome to become dysfunctional and progress to chronic gut issues. Other research studies have shown that environmental factors also play a role in altering the gut microbiome. These factors cause unwanted changes that can harm a person without even knowing. Figuring out which factors affect the gut can be prevented when a person puts in the work to better their health.
Conclusion
As stated earlier in today’s article, the gut microbiome is considered the largest endocrine organ that helps metabolize the immune system and homeostasis in the body. Therefore, replenishing the gut microbiome with beneficial bacteria can help solve the majority of chronic issues affecting the body. When environmental factors cause havoc to the gut system, it can affect the entire body if it is not treated right away. Eliminating the harmful environmental elements from a person’s daily lifestyle can provide the much-needed relief they have been searching for.
References
Al Bander, Zahraa, et al. “The Gut Microbiota and Inflammation: An Overview.” International Journal of Environmental Research and Public Health, MDPI, 19 Oct. 2020, www.ncbi.nlm.nih.gov/pmc/articles/PMC7589951/.
Durack, Juliana, and Susan V Lynch. “The Gut Microbiome: Relationships with Disease and Opportunities for Therapy.” The Journal of Experimental Medicine, Rockefeller University Press, 7 Jan. 2019, www.ncbi.nlm.nih.gov/pmc/articles/PMC6314516/.
Ferraris, Cinzia, et al. “Gut Microbiota for Health: How Can Diet Maintain a Healthy Gut Microbiota?” Nutrients, MDPI, 23 Nov. 2020, www.ncbi.nlm.nih.gov/pmc/articles/PMC7700621/.
Lobionda, Stefani, et al. “The Role of Gut Microbiota in Intestinal Inflammation with Respect to Diet and Extrinsic Stressors.” Microorganisms, MDPI, 19 Aug. 2019, www.ncbi.nlm.nih.gov/pmc/articles/PMC6722800/.
Thursby, Elizabeth, and Nathalie Juge. “Introduction to the Human Gut Microbiota.” The Biochemical Journal, Portland Press Ltd., 16 May 2017, www.ncbi.nlm.nih.gov/pmc/articles/PMC5433529/.
Disclaimer
Disclaimers
Professional Scope of Practice *
The information herein on "How To Diversify Your Digestive System" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's wellness blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-C) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on dralexjimenez.com, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card