“For individuals experiencing pelvis pain symptoms and associated problems, can integrating pelvic floor physical therapy exercises help with treatment and prevention?”
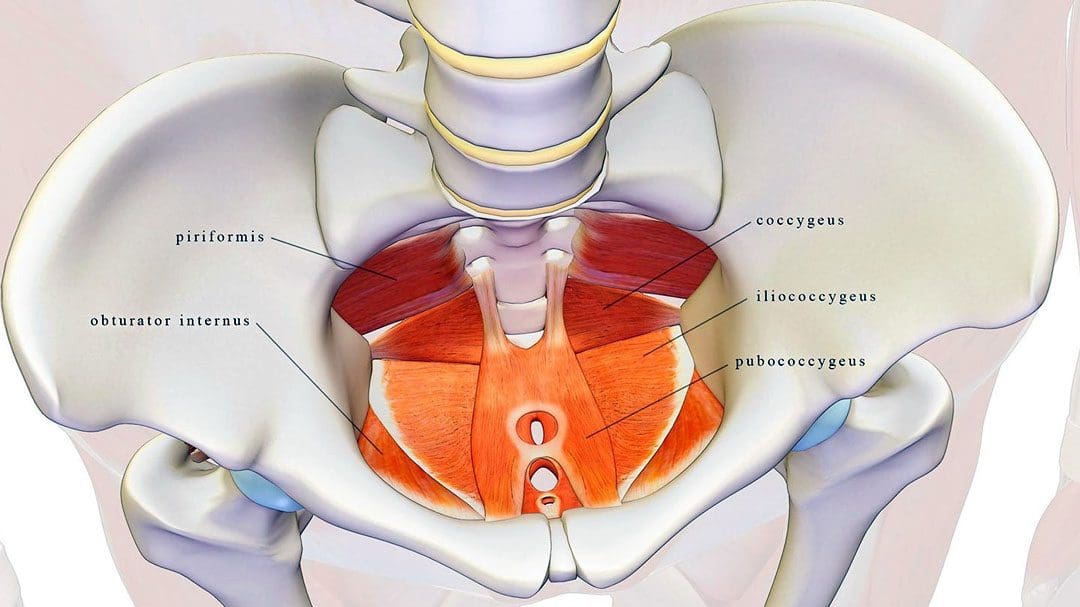
Table of Contents
Pelvic Floor Physical Therapy
- The pelvic floor muscles are located at the base of the pelvis and protect the pelvic organs like the vagina, cervix, uterus, bladder, urethra, and rectum. (U.S. Food and Drug Administration. 2019)
- They provide posture support, aid in orgasm function, facilitate sphincter function, and help pump lymphatic blood. (Dulcegleika Vilas Boas Sartori, et al., 2021) (Varuna Raizada, Ravinder K. Mittal. 2008)
When the muscles fail to function correctly, individuals can experience symptoms like:
- Painful intercourse
- Prolapse – when an organ or tissue drops or shifts out of place.
- Urinary incontinence
- Constipation problems
- These conditions are common in pregnant individuals or older women.
These symptoms can be treated with pelvic floor physical therapy to alleviate discomfort. Pelvic floor physical therapy can help women and individuals with vaginas:
- Alleviate issues like painful sex, urinary leakage, and prolapse.
- In physical therapy, individuals work on breathing, relaxation, and lengthening and strengthening techniques to train their muscles to function optimally.
Causes of Pelvic Floor Issues
Pelvic floor dysfunction tends to happen with age, during pregnancy, or in combination with events like the postpartum period and menopause, which can lower hormone levels.
- Individuals who are pregnant are especially prone to pelvic floor issues but might not know they have a problem.
- The pregnancy weight of a uterus can pressure and strain the muscles.
- Vaginal childbirth can also stretch or weaken the muscles. (Ilaria Soave, et al., 2019)
Symptoms
Symptoms can include: (Columbia Surgery. 2022)
- Pain in the pelvis region
- Back pain
- Painful urination
- Constipation
- Urinary leakage or incontinence
- Stool leakage or incontinence
- Painful intercourse
- If left untreated, these symptoms can worsen over time.
Pelvic Floor Physical Therapy
An individual will meet with a specialist to discuss symptoms and undergo a physical examination that includes:
- Pelvic floor exam.
- Evaluation of posture, mobility, and core strength.
- Once the initial exams and evaluation are complete, the practitioner will go over pelvic floor exercises and provide a treatment plan.
- Recommended exercises vary based on symptoms but focus on relaxing, stretching, and/or strengthening muscles.
Muscle Relaxation
- To relax the muscles, a therapist may recommend breathing exercises.
- For pregnant individuals, this means timing breaths with contractions.
- For individuals experiencing constipation, breathing exercises can help the body relax and reduce strain.
Stretching Muscles
- Stretching can help relieve muscle tightness and stiffness.
- A therapist may help stretch the pelvic floor through various therapy modalities.
- This type of physical therapy can help loosen tight muscles or help gently reset dislocated organs back into place.
Strengthening Muscles
- After the pelvic floor is loose and relaxed, the focus typically switches to strengthening the muscles.
- Strength work may target abdominal muscles or the pelvic floor muscles themselves.
With time, commitment, and targeted treatment, individuals can use pelvic floor physical therapy to loosen tissues, strengthen muscles, and restore function.
Spinal Decompression In Depth
References
U.S. Food and Drug Administration. (2019). Pelvic organ prolapse (pop).
Sartori, D. V. B., Kawano, P. R., Yamamoto, H. A., Guerra, R., Pajolli, P. R., & Amaro, J. L. (2021). Pelvic floor muscle strength is correlated with sexual function. Investigative and clinical urology, 62(1), 79–84. doi.org/10.4111/icu.20190248
Raizada, V., & Mittal, R. K. (2008). Pelvic floor anatomy and applied physiology. Gastroenterology clinics of North America, 37(3), 493–vii. doi.org/10.1016/j.gtc.2008.06.003
Soave, I., Scarani, S., Mallozzi, M., Nobili, F., Marci, R., & Caserta, D. (2019). Pelvic floor muscle training for prevention and treatment of urinary incontinence during pregnancy and after childbirth and its effect on urinary system and supportive structures assessed by objective measurement techniques. Archives of gynecology and obstetrics, 299(3), 609–623. doi.org/10.1007/s00404-018-5036-6
Columbia Surgery. (2022). Pelvic floor disorders: frequently asked questions.
Disclaimers
Professional Scope of Practice *
The information herein on "Recognizing & Treating Pelvic Floor Dysfunction" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's wellness blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-C) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on dralexjimenez.com, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card