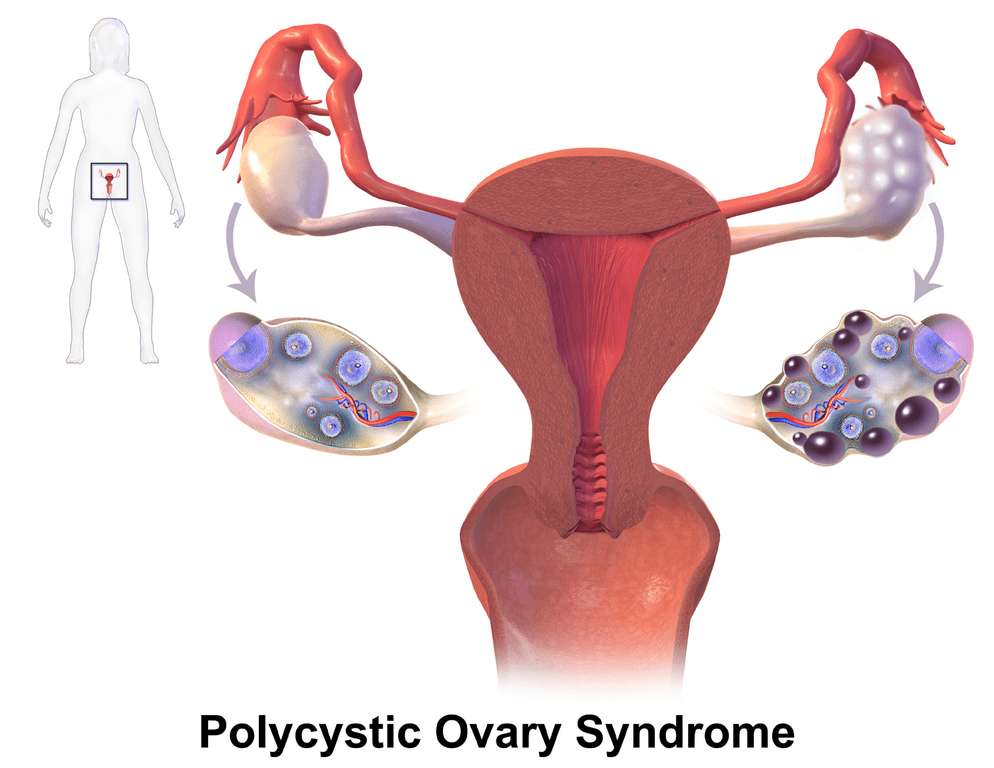
The prevalence of PCOS in women of reproductive age varies but has been reported to be around 6%-19% of this population. This condition’s etiology relies on the presence of multiple signs and symptoms like hyperandrogenism, chronic oligo-/anovulation, and insulin resistance. Nevertheless, these alterations’ presentation converges with the complexity of the patient’s genetic predisposition and the interactions with the environment.
A woman’s genetic predisposition combined with environmental factors such as a sedentary lifestyle and a diet constituted by high carbohydrate load, industrialized foods, and high saturated fat content is considered the triggers of this dysregulation. The initial androgen overproduction leads to reduced sized ovarian follicles, which results in an oligo-/anovulation problem. The lack of progesterone peaks modifies the GnRH dynamic, leading to a higher LH secretion, which stimulates the ovaries’ androgen synthesis. Furthermore, the ingestion of an unbalanced diet increased body weight, and insulin resistance leads to increased insulin secretion and a low-grade inflammatory milieu.
Table of Contents
Genetic studies and anthropology:
To understand how scientists discovered genetic information that ties PCOS and insulin resistance with human evolution is essential to look at what we were doing in prehistoric times.
The similarity of PCOS’s prevalence between different human populations shows that the genetic risk factors were present since our ancestors migrated from Africa. Furthermore, the human species come from an evolutionary path that can be traced back to chimpanzees, around 6 million years ago. Nevertheless, 50,000 years ago, anthropologists reported several human anatomy changes, describing them and a more modern, lean-bodied individual. In addition to these anatomical findings, brain size, body shape, increased fat storage, muscle, bone strength, new communication skills, and tools can be associated with a shift in diet and, therefore, metabolic changes. These findings are linked to the environmental conditions reported with a hunter-gatherer lifestyle.
If we fast forward to 40,000-10,000 years ago, we would observe a different environment. It has been reported that our ancestors went through another shift that accompanied a major dispersal of humans out of Africa and new stone-tools that allowed them to inhabit different geographic areas. Nevertheless, this was a harsh time for this population; child mortality was high; women died before turning 40 and were encouraged to have additional children at early ages. This wouldn’t last long after the hunter-gatherer approach came the agricultural period (10,000 years ago) along with a sedentary lifestyle. In fact, this would have an impact on women. Better nutrition and more food availability would result in early menarche and a longer period of fertility, fewer miscarriages, and lower child mortality.
Nowadays, the genome-wide association study (GWAS) provided the first PCOS research made in Chinese women, resulting in the identification of 3 susceptibility loci in the genes LHCGR, THADA, and DENND1A. Shortly after that, 8 new loci were found, and single-nucleotide polymorphisms (SNPs) in different genes code for hormones and growth. Conversely, these genes were similar to the ones related to type 2 diabetes. In fact, the effects of these loci have been found in women of European ancestry. This last finding shows that the genetic susceptibility of PCOS can be represented with the same loci and that the same PCOS genetic profile could be found across different ethnic groups.
GWAS
| Genes | Loci |
| LHCGR
THADA DENND1A C9orf3 FSHR INSR HMAGA2 YAP1 RAB2B/SOUX TOX3 SUMO1P1 |
2p16.3
2p21 9q33.1 9q22.32 11q22.1 12q13.2 12q14.3 16q12.1 19p13.3 20q13.2
|
Hyperandrogenemia and its protective effects:
The presence of high levels of androgens secreted by the adrenals in prehistoric women seems to point to the most common autosomal recessive genetic disorder, the nonclassic congenital adrenal hyperplasia (NCAH). This particular condition could be associated with early puberty and masculinization, protecting the women and their children given the cruel setting in which they lived. Also, women would have increased bone density, muscular strength, and mass, which would result in a feature for evolutionary matters.
On the other hand, cortisol might have had an additional resource for survival. It has been demonstrated that the secretion of cortisol in CYP21A heterozygote carriers of 21-hidroxylase deficiency could be protective against exacerbated immune responses and could improve homeostasis restoration in an inflammatory setting.
Insulin Resistance:
INSR codes for the insulin receptor have an important role in regulating insulin functions and have a tight association with PCOS genetic etiology. In fact, this gene has been passed through evolutionary phases. It is believed that the organization of insulin action/resistance is adapted from the famine and feast phases of our ancestors, from the hunter-gatherer era. During prolonged starvation, insulin resistance’s role is to minimize protein losses by reducing the necessity to utilize amino acid carbon skeletons to produce glucose.
Know your genes, know your treatment.
Studies in PCOS have shown that the loci and genes have not changed over 50 000 years. It is a fact that it has taken a toll on our feminine population. If we look into history, we could see that it was the body trying to protect us and ensure the race’s survival. Nevertheless, it is safe to say that what has changed is our lifestyle. I don’t know if you notice, but if these genes have been on our code for so long, our environment and lifestyle are the only things to modify.
Your daily methylation smoothie:
To ensure my daily fiber and veggie intake, I like to start strong. Most of the days, this is my favorite smoothie to have as part of my breakfast.
Ginger Greens Juice Servings: 1
• 1 cup pineapple cubes ( I cut mine in advance)
• 1/2 frozen blackberries or strawberries
• 1-inch knob of ginger, rinsed, peeled, and chopped
• 3 cups kale, rinsed and roughly chopped or ripped or nopal (which I love. It makes everything sticky. Add more water).
-Ana Paola RodrÃguez Arciniega. Master in Clinical Nutrition
References
Ãœnlütürk, UÄŸur, Efe Sezgin, and Bulent Okan Yildiz. “Evolutionary determinants of polycystic ovary syndrome: part 1.” Fertility and sterility 106.1 (2016): 33-41.
Dr. Alex Jimenez’s Blog Post
Disclaimer
Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the musculoskeletal system’s injuries or disorders. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas*& New Mexico*Â
Disclaimers
Professional Scope of Practice *
The information herein on "PCOS: A Genetic Predisposition-Part 1" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's wellness blog, where Dr. Alex Jimenez, DC, FNP-C, a board-certified Family Practice Nurse Practitioner (FNP-C) and Chiropractor (DC), presents insights on how our team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on dralexjimenez.com, focusing on restoring health naturally for patients of all ages.
Our areas of chiropractic practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is limited to chiropractic, musculoskeletal, physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system.
Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.*
Our office has reasonably attempted to provide supportive citations and has identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: coach@elpasofunctionalmedicine.com
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License # TX5807
New Mexico DC License # NM-DC2182
Licensed as a Registered Nurse (RN*) in Texas & Multistate
Texas RN License # 1191402
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card






